Analysis on death cause and life loss of malignant tumor in Wuhai from 2015 to 2018
-
摘要:
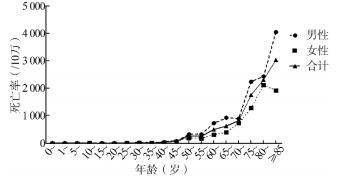
目的 分析乌海市居民恶性肿瘤死亡分布特点,为制定相应干预措施提供依据。 方法 根据2015—2018年乌海市居民死亡资料,计算恶性肿瘤死亡率、死因构成、死因顺位及寿命损失指标等。 结果 乌海市居民男性、女性和合计恶性肿瘤死亡率分别为199.66/10万、122.99/10万和163.02/10万,标化死亡率分别为216.47/10万、142.68/10万和180.45/10万,男女性别比为1.52:1。男性和女性的前3位恶性肿瘤死因均为肺癌、胃癌和肝癌。15~岁组死亡率最低(2.46/10万);而85~岁组死亡率最高(3 042.28/10万)。14岁以前主要恶性肿瘤死因为白血病,15岁以后为肺癌、胃癌和肝癌。恶性肿瘤导致的潜在减寿年数(potential years of life lost,PYLL)占全死因的46.9%,男性和女性中均为肺癌最高;男性平均减寿年数(average years of life lost,AYLL)最高是肝癌,女性最高是乳腺癌,其次为宫颈癌。 结论 恶性肿瘤已经成为乌海市居民的主要致死原因之一,肺癌、胃癌和肝癌是严重危害乌海市居民健康的恶性肿瘤死因,也应重点防治女性乳腺癌和宫颈癌的发生。应有针对地开展提高居民健康水平的健康教育工作。 Abstract:Objective To analyze the characteristics of malignant tumor death distribution of residents in Wuhai City, and to provide basis for formulating corresponding intervention measures. Methods According to the death data of residents in Wuhai City from 2015 to 2018, the mortality rate, the constituent ratio of death cause, the order of death causes and the indicators of life loss of malignant tumors were calculated. Results The mortality rates of male, female and total malignant tumor were 199.66/100 000, 122.99/100 000 and 163.02/100 000 respectively, and the standard mortality rates were 216.47/100 000, 142.68/100 000 and 180.45/100 000 respectively. Ratio of male to female was 1.52:1. The top three causes of death for men and women were lung cancer, stomach cancer and liver cancer. The lowest mortality rate was 2.46/100 000 in the aged 15 to 19 years, while the highest mortality rate was 3042.28/100 000 in the aged 85 years or above. The major cause of malignancy death in aged before 14 years was leukemia, and in aged after 15 years was lung cancer, stomach cancer and liver cancer. Potential years of life lost (PYLL) caused by malignancy accounted for 46.9% of all, and lung cancer was the highest among both men and women. Average years of life lost (AYLL) showed that liver cancer was the highest in men and breast cancer in women, followed by cervical cancer. Conclusions Malignant tumor has become one of the main causes of death for residents of Wuhai City. Lung cancer, stomach cancer and liver cancer are the causes of death of malignant tumors that seriously endanger the health of residents in Wuhai City. In addition, the prevention and treatment of female breast cancer and cervical cancer should also be emphasized. There should be targeted work to reduce malignant tumor mortality and improve the health of residents. -
Key words:
- Death surveillance /
- Malignant tumor /
- Mortality rate /
- Loss of life
-
表 1 2015—2018年乌海市居民恶性肿瘤主要死因顺位
Table 1. Rank order of causes of death of malignant tumors in Wuhai residents from 2015 to 2018
死因
顺位男性 女性 合计 死因 死亡人数 构成比(%) 死亡率(/10万) 死因 死亡人数 构成比(%) 死亡率(/10万) 死因 死亡人数 构成比(%) 死亡率(/10万) 1 肺癌 740 31.9 63.68 肺癌 309 23.62 29.06 肺癌 1 049 28.91 47.14 2 胃癌 367 15.82 31.58 胃癌 145 11.09 13.63 胃癌 512 14.11 23.01 3 肝癌 309 13.32 26.59 肝癌 143 10.93 13.45 肝癌 452 12.46 20.31 4 食管癌 133 5.73 11.45 乳腺癌 98 7.49 9.22 食管癌 173 4.77 7.77 5 结肠癌 80 3.45 6.88 宫颈癌 66 5.05 6.21 胰腺癌 133 3.67 5.98 6 直肠癌 78 3.36 6.71 胰腺癌 63 4.82 5.92 结肠癌 132 3.64 5.93 7 胰腺癌 70 3.02 6.02 结肠癌 52 3.98 4.89 直肠癌 125 3.45 5.62 8 膀胱癌 53 2.28 4.56 直肠癌 47 3.59 4.42 乳腺癌 99 2.73 4.45 9 前列腺癌 37 1.59 3.18 食管癌 40 3.06 3.76 宫颈癌 66 1.82 2.79 10 胆囊癌 32 1.38 2.75 卵巢癌 32 2.45 3.01 膀胱癌 64 1.76 2.88 合计 1 899 81.85 163.43 995 76.07 93.56 2 805 77.32 126.04 表 2 2015—2018年乌海市居民不同年龄组恶性肿瘤主要死因顺位
Table 2. Rank order of causes of death of malignant tumors in different age groups of Wuhai residents
死因
顺位0~岁 15~岁 40~岁 ≥65岁 死因 构成比(%) 死亡率(/10万) 死因 构成比(%) 死亡率(/10万) 死因 构成比(%) 死亡率(/10万) 死因 构成比(%) 死亡率(/10万) 1 淋巴样白血病 27.78 1.81 胃癌 18.95 1.99 肺癌 25.39 41.54 肺癌 32.15 356.66 2 未特指类型白血病 27.78 1.81 肝癌 15.79 1.66 肝癌 16.79 27.46 胃癌 14.19 157.41 3 脑脊膜癌 11.11 0.73 肺癌 13.68 1.43 胃癌 13.85 22.65 肝癌 9.57 106.16 4 脑癌 11.11 0.73 白血病 9.47 0.99 乳腺癌 4.66 7.63 食管癌 5.42 60.14 5 其他和不明部位癌 5.56 0.36 乳腺癌 6.32 0.66 食管癌 4.02 6.57 直肠癌 4.34 48.11 6 弥漫性非霍奇金淋巴癌 5.56 0.36 脑癌 4.21 0.44 结肠癌 3.44 5.63 胰腺癌 4.01 44.45 7 多发性骨髓瘤和恶性浆细胞肿瘤 5.56 0.36 淋巴、造血其他癌 3.16 0.33 胰腺癌 3.3 5.4 结肠癌 3.82 42.36 8 淋巴、造血和有关组织其他额
未特指的癌5.56 0.36 结肠癌 3.16 0.33 宫颈癌 2.94 4.81 膀胱癌 2.45 27.19 9 胆囊癌 3.16 0.33 直肠癌 2.3 3.75 前列腺癌 1.6 17.78 10 宫颈癌 3.16 0.33 胆囊癌 1.79 2.93 乳腺癌 1.32 14.64 合计 100 6.53 81.05 8.50 78.48 128.37 78.88 879.91 表 3 2015—2018年乌海市居民主要恶性肿瘤死因寿命损失分析
Table 3. Analysis of life loss of major malignant tumors in Wuhai residents from 2015 to 2018
死因
顺位男性 女性 合计 肿瘤
类型PYLL
(人年)PYLLR
(‰)SPYLL
(人年)SPYLLR
(‰)AYLL
(年)肿瘤
类型PYLL
(人年)PYLLR
(‰)SPYLL
(人年)SPYLLR
(‰)AYLL
(年)肿瘤
类型PYLL
(人年)PYLLR
(‰)SPYLL
(人年)SPYLLR
(‰)AYLL
(年)1 肺癌 5 143 4.43 4 836 4.16 6.95 肺癌 3 308 3.11 2 787 2.62 10.71 肺癌 9 276 4.17 4 215 1.89 8.84 2 肝癌 4 657 4.01 4 511 3.88 15.17 乳腺癌 2 290 2.15 2 136 2.01 23.37 肝癌 6 439 2.89 3 152 1.42 14.25 3 胃癌 3 038 2.61 2 739 2.36 8.28 胃癌 2 111 1.98 1 727 1.62 14.56 胃癌 5 819 2.61 2 629 1.18 11.37 4 食管癌 857 0.74 760 0.65 6.44 肝癌 1 474 1.39 1 240 1.17 10.31 乳腺癌 2 070 0.93 987 0.44 20.91 5 胰腺癌 729 0.63 673 0.58 10.41 宫颈癌 1 384 1.30 1 216 1.14 20.97 胰腺癌 1 401 0.63 637 0.29 10.53 全恶性肿瘤死因 20 749 17.86 19 683 16.94 8.94 17 285 16.25 14 990 14.1 13.21 40 463 18.18 18 369 16.17 11.15 -
[1] Lindsey A, Freddie Bray, Rebecca L, et al. Global cancer statistics, 2012[J]. CA Cancer J Clin, 2015, 65(2):87-108. DOI: 10.3322/caac.21262. [2] Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018:Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2018, 68(6):394-424. DOI: 10.3322/caac.21492. [3] International agency for research on cancer. Cancer Today[EB/OL]. (2019-06-19)[2020-02-15].http://gco.iarc.fr/today/online-analysis. [4] 国家卫生和计划生育委员会统计信息中心, 中国疾病预防控制中心慢性非传染性疾病预防控制中心.中国死因监测数据集2016[M].北京:中国科学技术出版社, 2017:26.National Health and Family Planning Commission Statistical Information Center, Chinese Center for Disease Control and Prevention Chronic Non-communicable Disease Prevention and Control Center. Chinese death cause monitoring data set 2016[M]. Beijing:China Science and Technology Press, 2017:26. [5] Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015[J]. CA Cancer J Clin, 2016, 66(2):115-132. DOI: 10.3322/caac.21338. [6] 郑荣寿, 李贺, 陈万青, 等. 2000-2014年中国肿瘤登记地区癌症发病趋势及年龄变化分析[J].中华预防医学杂志, 2018, 52(6):593-600. DOI: 10.3760/cma.j.issn.0253-9624.2018.06.007.Zheng RS, Li H, Chen WQ, et al. Analysis on the trend of cancer incidence and age change in cancer registry areas of China, 2000 to 2014[J]. Chin J Prev Med, 2018, 52(6):593-600. DOI: 10.3760/cma.j.issn.0253-9624.2018.06.007. [7] Cai Y, Xue M, Chen W, et al. Expenditure of hospital care on cancer in China, from 2011 to 2015[J]. Chin J Cancer Res, 2017, 29(3):253-262. DOI: 10.21147/j.issn.1000-9604.2017.03.11. [8] Islami F, Chen W, Yu XQ, et al. Cancer deaths and cases attributable to lifestyle factors and infections in China, 2013[J]. Ann Oncol, 2017, 28(10):2567-2574. DOI: 10.1093/annonc/mdx34. [9] 孙雯雯. 2016年抚顺市城市居民死因监测分析[J].中国卫生统计, 2018, 35(3):457-458,461. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgwstj201803036Sun WW. Monitoring and analysis of the causes of death of urban residents in Fushun in 2016[J]. Chin J Health Statistics, 2018, 35(3):457-458,461. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=zgwstj201803036 [10] 饶裕莲.南昌市湾里区2014-2017年居民死因监测与疾病负担分析[D].南昌: 南昌大学, 2019.Rao YL. Study on the death causes and its burden of disease for residents in Wali district of Nanchang City from 2014 to 2017[D]. Nanchang: Nanchang University, 2019. [11] 马麟, 桑志宏, 于颖洁, 等. 2017年山西省死因监测点居民死因监测分析[J].中国药物与临床, 2019, 19(4):655-657. DOI: 10.11655/zgywylc2019.04.059.Ma L, Sang ZH, Yu YJ, et al. Analysis on the monitoring of death causes of residents in Shanxi province in 2017[J]. Chinese Remedies & Clinics, 2019, 19(4):655-657. DOI: 10.11655/zgywylc2019.04.059. [12] 郑荣寿, 孙可欣, 张思维, 等. 2015年中国恶性肿瘤流行情况分析[J].中华肿瘤杂志, 2019, 41(1):19-28. DOI: 10.3760/cma.j.issn.0253-3766.2019.01.005.Deng HR, Sun KX, Zhang SW, et al. Report of cancer epidemiology in China, 2015[J]. Chin J Oncol, 2019, 41(1):19-28. DOI: 10.3760/cma.j.issn.0253-3766.2019.01.005. [13] 张小燕, 陈鑫, 高磊, 等. 2010-2014年南京市浦口区居民恶性肿瘤死因及减寿分析[J].现代预防医学, 2017, 44(8):169-172. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=xdyfyx201708037Zhang XY, Chen X, Gao L, et al. Analysis of the death causes of malignant tumors and reduction of life expectancy among residents in Pukou district in Nanjing City between 2010 and 2014[J]. Modern Preventive Medicine, 2017, 44(8):169-172. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=xdyfyx201708037 [14] 黄春妍, 王临池, 陆艳, 等. 1987-2017年苏州市恶性肿瘤死亡流行特征及变化趋势[J].中国肿瘤, 2020, 29(2):90-95. DOI: 10.11735/j.issn.1004-0242.2020.02.A002.Huang CY, Wang LC, Lu Y. et al. Epidemiological characteristics and trend of cancer mortality in Suzhou from 1987 to 2017[J]. China Cancer, 2020, 29(2):90-95. DOI: 10.11735/j.issn.1004-0242.2020.02.A002. [15] 王莹, 宫舒萍, 高昌, 等. 2011-2017年济南市居民死因分析及疾病负担研究[J].中国慢性病预防与控制, 2019, 27(6):468-471. DOI: 10.16386/j.cjpccd.issn.1004-6194.2019.06.018.Wang Y, Gong SP, Gao C, et al. Jinan city resident cause analysis and disease burden study from 2011 to 2017[J]. Chin J Prev Contr Chron Dis, 2019, 27(6):468-471. DOI: 10.16386/j.cjpccd.issn.1004-6194.2019.06.018. [16] 金头峰, 全贞玉. 2000年与2010年延吉市居民恶性肿瘤死因比较分析[J].现代预防医学, 2015, 42(19):3599-3601. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=xdyfyx201519044Jin TF, Quan ZY. Comparison of malignant tumors of residents in Yanji City in 2000 and 2010[J]. Modern Preventive Medicine, 2015, 42(19):3599-3601. http://www.wanfangdata.com.cn/details/detail.do?_type=perio&id=xdyfyx201519044 [17] 李燕, 张嫣平, 刘兰. 2011-2015年宁夏银川市居民恶性肿瘤死因及减寿分析[J].中华疾病控制杂志, 2017, 21(10):997-1001. DOI: 10.16462/j.cnki.zhjbkz.2017.10.007.Li Y, Zhang YP, Liu L. Analysis on mortality and PYLL of malignant tumor in Yinchuan of Ningxia Province from 2011 to 2015[J]. Chin J Dis Control Prev, 2017, 21(10):997-1001. DOI: 10.16462/j.cnki.zhjbkz.2017.10.007. [18] 姜申易, 吴彬, 于晓松.中国2004-2015年城乡女性恶性肿瘤死因顺位及死亡率分析[J].中国公共卫生, 2019, 35(12):1706-1709. DOI: 10.11847/zgggws1122648.Jiang SY, Wu B, Yu XS. Malignant tumor mortality and rank order of death among urban and rural female residents in China:2004—2015[J]. Chin J Publ Heal, 2019, 35(12):1706-1709. DOI: 10.11847/zgggws1122648. -





 下载:
下载: