Study on the association between pulse pressure and renal function decline among middle-aged and elderly people
-
摘要:
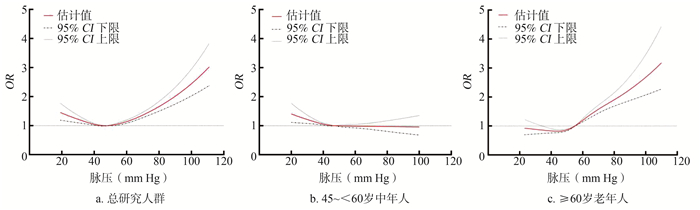
目的 探讨中老年人脉压(pulse pressure, PP)与肾功能下降的关系。 方法 以2015年1月1日—2019年12月31日在重庆医科大学附属第一医院参加健康体检的46 605例中老年人(≥45岁)为研究对象,按其PP水平分为四组(< 40 mm Hg、40~ < 50 mm Hg、50~ < 60 mm Hg、≥60 mm Hg),采用非条件Logistic回归分析模型分析PP与肾功能下降的关联。 结果 本研究46 605例中老年人年龄为54(48, 60)岁,肾功能下降者占27.37%(其中轻度占26.45%,中重度占0.92%)。与同年龄人群对照组相比,PP < 40 mm Hg和PP≥60 mm Hg组中老年人发生肾功能下降的风险分别升高11%和28%;按年龄分层后,45~ < 60岁中年人仅PP < 40 mm Hg组发生肾功能下降的风险升高13%(OR=1.13, 95% CI: 1.05~1.22),≥60岁老年人PP为50~ < 60 mm Hg和PP≥60 mm Hg组发生肾功能下降的风险分别升高12%(OR=1.12, 95% CI: 1.02~1.24)和66%(OR=1.66, 95% CI: 1.48~1.86)。限制性立方样条结果提示PP与肾功能下降的关联强度呈非线性关系,中年人PP < 42 mm Hg,老年人PP>55 mm Hg时肾功能下降风险增加。PP与肾功能下降程度关联分析结果显示,中年人仅PP < 40 mm Hg组发生肾功能轻度下降的风险升高13%(OR=1.13, 95% CI: 1.05~1.22);老年人PP为50~ < 60 mm Hg组发生肾功能轻度下降的风险升高11%(OR=1.11, 95% CI: 1.01~1.23),PP≥60 mm Hg组发生肾功能轻度和中重度下降的风险分别升高61%(OR=1.61, 95% CI: 1.43~1.81)和179%(OR=2.79, 95% CI: 1.94~4.02)。 结论 PP对肾功能下降及下降程度发生风险的影响在中年人和老年人中并不相同,应特别关注PP减小的中年人和PP增大的老年人的肾功能情况。 Abstract:Objective To explore the association between pulse pressure (PP) and renal function decline among middle-aged and elderly people. Methods A total of 46 605 middle-aged and elderly people (aged ≥45 years old) who participated in the physical examination in the First Affiliated Hospital of Chongqing Medical University from January 1, 2015 to December 31, 2019 were selected as the study objects. According to their PP levels, they were divided into four groups (PP < 40 mm Hg, 40- < 50 mm Hg, 50- < 60 mm Hg, and ≥60 mm Hg). Unconditional Logistic regression model was used to analyze the association between PP and renal function decline. Results The age of the 46 605 people included in this study was 54(48, 60) years old, and 27.37% of them had renal function decline (26.45% were mild, and 0.92% were moderate-severe). Compared with the same age group, the risk of renal function decline increased by 11% and 28% in PP < 40 mm Hg and PP≥60 mm Hg groups among middle-aged and elderly people, respectively. The results of age stratification analysis showed that among middle-aged people aged 45- < 60 years old, the risk of renal function decline increased by 13% (OR=1.13, 95% CI: 1.05-1.22) only in the PP < 40 mm Hg group, while among elderly people aged ≥60 years old, the risk increased by 12% (OR=1.12, 95% CI: 1.02-1.24) and 66% (OR=1.66, 95% CI: 1.48-1.86) in the PP=50- < 60 mm Hg and PP≥60 mm Hg groups, respectively. Restrictive cubic spline results suggested that the association between PP and renal function decline was non-linear, and the risk of renal function decline increased when PP < 42 mm Hg in middle-aged people and PP>55 mm Hg in elderly people. The results of correlation analysis between PP and different degrees of renal function decline showed that the risk of mild renal function decline was increased by 13% (OR=1.13, 95% CI: 1.05-1.22) only in middle-aged people with PP < 40 mm Hg group, while the risk of mild renal function decline was increased by 11%(OR=1.11, 95% CI: 1.01-1.23) in elderly people with PP=50- < 60 mm Hg group, and the risk of mild and moderate-severe renal function decline was increased by 61%(OR=1.61, 95% CI: 1.43-1.81)and 179%(OR=2.79, 95% CI: 1.94-4.02) in elderly people with PP≥60 mm Hg group, respectively. Conclusions The effect of PP on the risk of renal function decline and its degrees was not the same in middle-aged people and elderly people. Special attention should be paid to the renal function of middle-aged people with decreased PP and elderly people with increased PP. -
表 1 研究对象基本特征比较[n(%)]
Table 1. The comparison of the basic characteristics of the study objects [n(%)]
变量 肾功能正常(n=33 851) 肾功能下降(n=12 754) χ2值 P值 体检年份(年) 186.03 < 0.001 2015 2 055(6.07) 794(6.23) 2016 5 188(15.33) 2 564(20.10) 2017 6 172(18.23) 2 402(18.83) 2018 8 101(23.93) 2 631(20.63) 2019 12 335(36.44) 4 363(34.21) 人群 4 435.66 < 0.001 中年人 27 883(82.37) 6 637(52.04) 老年人 5 968(17.63) 6 117(47.96) 性别 576.52 < 0.001 男 17 801(52.59) 8 287(64.98) 女 16 050(47.41) 4 467(35.02) 超重/肥胖 87.57 < 0.001 否 19 047(56.56) 6 558(51.71) 是 14 626(43.44) 6 124(48.29) 高血压 309.82 < 0.001 否 26 260(77.58) 8 889(69.70) 是 7 591(22.42) 3 865(30.30) 糖尿病 29.00 < 0.001 否 31 465(94.05) 12 011(95.35) 是 1 991(5.95) 586(4.65) 血脂异常 17.60 < 0.001 否 22 223(66.01) 8 104(63.92) 是 11 445(33.99) 4 574(36.08) PP(mm Hg) 647.56 < 0.001 < 40 5 534(16.35) 1 719(13.48) 40~ < 50 13 694(40.45) 4 284(33.59) 50~ < 60 9 694(28.64) 3 685(28.89) ≥60 4 929(14.56) 3 066(24.04) 表 2 中老年人脉压与肾功能下降的多因素Logistic回归分析模型分析
Table 2. Multivariate Logistic regressive model analysis of the association between pulse pressure and renal function decline in middle-aged and elderly people
人群 PP (mm Hg) 单因素分析 多因素分析 OR(95% CI)值 P值 ORa(95% CI)值 P值 中老年人(n=46 605) 40~49 1.00 1.00 < 40 0.99(0.93~1.06) 0.828 1.11(1.04~1.19) 0.003 50~ < 60 1.22(1.15~1.28) < 0.001 1.02(0.96~1.07) 0.583 ≥60 1.99(1.88~2.10) < 0.001 1.28(1.18~1.37) < 0.001 中年人(n=34 520) 40~49 1.00 1.00 < 40 1.11(1.03~1.19) 0.007 1.13(1.05~1.22) 0.001 50~ < 60 0.97(0.91~1.04) 0.394 0.99(0.92~1.06) 0.729 ≥60 0.89(0.81~0.97) 0.012 0.96(0.86~1.07) 0.425 老年人(n=12 085) 40~49 1.00 1.00 < 40 0.94(0.80~1.09) 0.401 0.94(0.80~1.10) 0.433 50~ < 60 1.06(0.96~1.16) 0.253 1.12(1.02~1.24) 0.023 ≥60 1.46(1.33~1.61) < 0.001 1.66(1.48~1.86) < 0.001 注:a调整因素为体检年份、年龄(总研究人群中调整)、性别、超重/肥胖、高血压、糖尿病、血脂异常。 表 3 中老年人脉压与不同程度肾功能下降的多因素Logistic回归分析模型分析
Table 3. Multivariate Logistic regression analysis of the association between pulse pressure and different degrees of renal function decline in middle-aged and elderly people
人群 PP (mm Hg) 肾功能轻度下降 肾功能中重度下降 OR(95% CI)值 P值 ORa(95% CI)值 P值 OR (95% CI)值 P值 ORa(95% CI)值 P值 中老年人(n=46 605) 40~ < 50 1.00 1.00 1.00 1.00 < 40 1.00(0.94~1.06) 0.947 1.11(1.04~1.19) 0.003 0.76(0.49~1.17) 0.212 0.95(0.62~1.47) 0.831 50~ < 60 1.20(1.14~1.26) < 0.001 1.01(0.96~1.07) 0.684 1.93(1.46~2.54) < 0.001 1.26(0.94~1.67) 0.117 ≥60 1.90(1.80~2.02) < 0.001 1.25(1.16~1.35) < 0.001 6.03(4.67~7.78) < 0.001 2.24(1.64~3.07) < 0.001 中年人(n=34 520) 40~ < 50 1.00 1.00 1.00 1.00 < 40 1.11(1.03~1.19) 0.007 1.13(1.05~1.22) 0.001 0.97(0.51~1.85) 0.928 1.07(0.56~2.04) 0.842 50~ < 60 0.97(0.91~1.03) 0.33 0.99(0.92~1.06) 0.703 0.97(0.80~2.23) 0.267 1.34(0.65~1.88) 0.711 ≥60 0.87(0.79~0.96) 0.004 0.95(0.85~1.05) 0.316 2.48(1.41~4.34) 0.002 1.57(0.82~3.01) 0.174 老年人(n=12 085) 40~ < 50 1.00 1.00 1.00 1.00 < 40 0.94(0.80~1.09) 0.433 0.94(0.80~1.11) 0.471 0.94(0.80~1.09) 0.599 0.85(0.47~1.54) 0.583 50~ < 60 1.06(0.96~1.16) 0.343 1.11(1.01~1.23) 0.037 1.06(0.96~1.16) 0.15 1.35(0.95~1.90) 0.091 ≥60 1.46(1.33~1.61) < 0.001 1.61(1.43~1.81) < 0.001 1.46(1.33~1.61) < 0.001 2.79(1.94~4.02) < 0.001 -
[1] 胡盛寿, 高润霖, 刘力生, 等. 《中国心血管病报告2018》概要[J]. 中国循环杂志, 2019, 34(3): 209-220. DOI: 10.3969/j.issn.1000-3614.2019.03.001.Hu SS, Gao RL, Liu LS, et al. Summary of the 2018 Report on Cardiovascular Diseases in China[J]. Chin Circ J, 2019, 34(3): 209-220. DOI: 10.3969/j.issn.1000-3614.2019.03.001. [2] 崔露露. 脉压的影响因素及其与靶器官损害的研究进展[J]. 海南医学, 2019, 30(10): 1336-1340. DOI: 10.3969/j.issn.1003-6350.2019.10.033.Cui LL. Influential factors of pulse pressure and its research progress on target organ damage[J]. Hainan Med J, 2019, 30(10): 1336-1340. DOI: 10.3969/j.issn.1003-6350.2019.10.033. [3] 王增武, 陈祚, 王芳, 等. 北京市某社区中老年人群肾功能下降与心血管事件的关联研究[J]. 中华流行病学杂志, 2010, 31(8): 841-844. DOI: 10.3760/cma.j.issn.0254-6450.2010.08.001.Wang ZW, Chen Z, Wang F, et al. Association between chronic kidney disease and cardiovascular events in middle-to-old-aged Chinese population[J]. Chin J Epidemiol, 2010, 31(8): 841-844. DOI: 10.3760/cma.j.issn.0254-6450.2010.08.001. [4] Zhang YP, Zuo XC, Huang ZJ, et al. The impact of blood pressure on kidney function in the elderly: a cross-sectional study[J]. Kidney Blood Press Res, 2013, 38(2-3): 205-216. DOI: 10.1159/000355769. [5] 侯金泓, 王剑利, 李俊娟, 等. 老年人基线脉压水平对远期肾功能的影响[J]. 中华老年心脑血管病杂志, 2014, 16(10): 1038-1040. DOI: 10.3969/j.issn.1009-0126.2014.10.009.Hou JH, Wang JL, Li JJ, et al. Effect of pulse pressure on long-term kidney function in the elderly[J]. Chin J Geriatr Heart Brain Vessel Dis, 2014, 16(10): 1038-1040. DOI: 10.3969/j.issn.1009-0126.2014.10.009. [6] Zhang L, Wang F, Wang L, et al. Prevalence of chronic kidney disease in China: a cross-sectional survey[J]. Lancet, 2012, 379(9818): 815-822. DOI: 10.1016/S0140-6736(12)60033-6. [7] 张钦凤, 朴鍾龜, 高尚伯, 等. 脉压与心脑血管病的关系: 一个大样本的随访研究[J]. 中华高血压杂志, 2006, 14(10): 830-832. DOI: 10.3969/j.issn.1673-7245.2006.10.017.Zhang QF, Park JK, Sang BK, et al. Relation between pulse pressure and cardio-cerebralvascular disease[J]. Chin J Hypertens, 2006, 14(10): 830-832. DOI: 10.3969/j.issn.1673-7245.2006.10.017. [8] Anderson RJ, Bahn GD, Emanuele NV, et al. Blood pressure and pulse pressure effects on renal outcomes in the Veterans Affairs Diabetes Trial (VADT)[J]. Diabetes Care, 2014, 37(10): 2782-2788. DOI: 10.2337/dc14-0284. [9] Peralta CA, Norris KC, Li S, et al. Blood pressure components and end-stage renal disease in persons with chronic kidney disease: the Kidney Early Evaluation Program (KEEP)[J]. Arch Intern Med, 2012, 172(1): 41-47. DOI: 10.1001/archinternmed.2011.619. [10] 中国肥胖问题工作组. 中国成人超重和肥胖症预防与控制指南(节录)[J]. 营养学报, 2004, 26(1): 1-4. DOI: 10.3321/j.issn:0512-7955.2004.01.001.Group of China Obesity Task Force. . Guidelines for the prevention and control of overweight and obesity in Chinese adults(excerpt)[J]. Acta Nutr Sin, 2004, 26(1): 1-4. DOI: 10.3321/j.issn:0512-7955.2004.01.001. [11] 《中国高血压防治指南》修订委员会. 中国高血压防治指南2018年修订版[J]. 心脑血管病防治, 2019, 19(1): 1-44. https://www.cnki.com.cn/Article/CJFDTOTAL-XIXG201901003.htmRevision Committee of the Guidelines for the Prevention and Treatment of Hypertension in China. China hypertension prevention and treatment guidelines 2018 revised edition[J]. Prev Treat Cardio-Cereb-Vasc Dis, 2019, 19(1): 1-44. https://www.cnki.com.cn/Article/CJFDTOTAL-XIXG201901003.htm [12] 中华医学会糖尿病学分会. 中国2型糖尿病防治指南(2017年版)[J]. 中国实用内科杂志, 2018, 38(4): 292-344. DOI: 10.19538/j.nk2018040108.Chinese Diabetes Society. Guidelines for the prevention and control of type 2 diabetes in China (2017 Edition)[J]. Chin J Pract Intern Med, 2018, 38(4): 292-344. DOI: 10.19538/j.nk201040108. [13] 诸骏仁, 高润霖, 赵水平, 等. 中国成人血脂异常防治指南(2016年修订版)[J]. 中国循环杂志, 2016, 31(10): 937-953. DOI: 10.3969/j.issn.1000-3614.2016.10.001.Zhu JR, Gao RL, Zhao SP, et al. Chinese guidelines for prevention and treatment of adult dyslipidemia (2016 revision)[J]. Chin Circ J, 2016, 31(10): 937-953. DOI: 10.3969/j.issn.1000-3614.2016.10.001. [14] Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate[J]. Ann Intern Med, 2009, 150(9): 604-612. DOI: 10.7326/0003-4819-150-9-200905050-00006. [15] 胡欢欢, 尹凤仙, 全贞玉, 等. 影响中老年健康体检人群肾小球滤过率的因素[J]. 中国老年学杂志, 2020, 40(10): 2116-2119. DOI: 10.3969/j.issn.1005-9202.2020.10.032.Hu HH, Yin FX, Quan ZY, et al. Factors affecting glomerular filtration rate in middle-aged and elderly healthy people[J]. Chin J of Gerontol, 2020, 40(10): 2116-2119. DOI: 10.3969/j.issn.1005-9202.2020.10.032. [16] Natali A, Boldrini B, Baldi S, et al. Impact of mild to moderate reductions of glomerular filtration rate on coronary artery disease severity[J]. Nutr Metab Cardiovasc Dis, 2014, 24(6): 681-688. DOI: 10.1016/j.numecd.2013.12.005. [17] 吴桂贤, 吴兆苏, 刘静, 等. 人群脉压分布特征的研究[J]. 中华心血管病杂志, 2001, 29(7): 55-59. DOI: 10.3760/j:issn:0253-3758.2001.07.025.Wu GX, Wu ZS, Liu J, et al. A cohort study of the distribution feature on pulse pressure[J]. Chin J Cardiol, 2001, 29(7): 55-59. DOI: 10.3760/j:issn:0253-3758.2001.07.025. [18] 杨建民, 路方红, 金世宽, 等. 中老年人脉压与脑卒中危险的相关性[J]. 中华高血压杂志, 2006, 14(9): 699-702. DOI: 10.16439/j.cnki.1673-7245.2006.09.006.Yang JM, Lu FH, Jin SK, et al. Pulse Pressure and Stroke[J]. Chin J Hypertens, 2006, 14(9): 699-702. DOI: 10.16439/j.cnki.1673-7245.2006.09.006. [19] 蒲国俭, 蒲世军. 中青年高血压315例临床分析[J]. 现代医药卫生, 2012, 28(23): 3561-3562. DOI: CNKI:SUN:XYWS.0.2012-23-022.Pu GJ, Pu SJ. Clinical analysis on 315 cases of young and middle-aged hypertension[J]. Mod Med Heal, 2012, 28(23): 3561-3562. DOI: CNKI:SUN:XYWS.0.2012-23-022. [20] 贡佳慧, 王国威, 卓琳, 等. 舒张压异常对肾功能的影响[J]. 中华高血压杂志, 2018, 26(7): 644-648. DOI: 10.16439/j.cnki.1673-7245.2018.07.017.Gong JH, Wang GW, Zhuo L, et al. The relationship between diastolic blood pressure and the decline of renal function[J]. Chin J Hypertens, 2018, 26(7): 644-648. DOI: 10.16439/j.cnki.1673-7245.2018.07.017. [21] Covic A, Gusbeth-Tatomir P, Goldsmith DJ. Arterial stiffness in renal patients: an update[J]. Am J Kidney Dis, 2005, 45(6): 965-977. DOI: 10.1053/j.ajkd.2005.02.026. [22] Pedrinelli R, Dell'Omo G, Penno G, et al. Microalbuminuria and pulse pressure in hypertensive and atherosclerotic men[J]. Hypertension, 2000, 35(1 Pt 1): 48-54. DOI: 10.1161/01.hyp.35.1.48. [23] Madero M, Peralta C, Katz R, et al. Association of arterial rigidity with incident kidney disease and kidney function decline: the Health ABC study[J]. Clin J Am Soc Nephrol, 2013, 8(3): 424-433. DOI: 10.2215/CJN.07900812. -





 下载:
下载: