-
摘要:
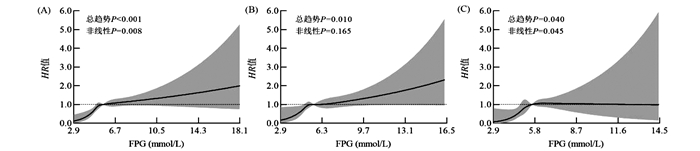
目的 了解金昌队列人群脑卒中的发病状况,探讨糖尿病及FPG与脑卒中发病之间的联系,为有效控制糖尿病、预防脑卒中的发生提供科学依据。 方法 以金昌队列为研究平台,采用前瞻性队列研究的方法分析糖尿病及FPG水平与脑卒中发病风险间的关系,运用限制样条法拟合FPG水平与脑卒中发病风险间的剂量反应关系。 结果 本研究共纳入32 736例研究对象,平均随访2.2年后,脑卒中累积发病率为8.77‰,其中糖尿病组脑卒中发病率为23.38‰,高于对照组发病率6.67‰。调整混杂因素后,糖尿病患者和空腹血糖受损人群中脑卒中的发病风险分别是对照组的2.257倍(HR=2.257, 95% CI: 1.658~3.072, P<0.001)和1.396倍(HR=1.396, 95% CI: 1.039~1.877, P=0.027)。以FPG < 5.6 mmol/L作为对照组,控制混杂因素后,总人群中FPG≥5.6 mmol/L组和FPG≥6.1 mmol/L组脑卒中的发病风险分别增加48.1%(HR=1.481, 95% CI: 1.040~2.108, P=0.030)和49.3%(HR=1.493, 95% CI: 1.044~2.136, P=0.028);当FPG≥7.0 mmol/L时,男性和女性脑卒中的发病风险分别是对照组的1.614倍(HR=1.614,95% CI: 1.068~2.438)和2.742倍(HR=2.742, 95% CI: 1.355~5.547)。在总人群和女性中FPG与脑卒中发病风险间呈非线性剂量反应关系,男性中FPG与脑卒中发病风险间呈线性剂量反应关系。 结论 糖尿病是脑卒中的独立危险因素,且FPG水平与脑卒中的发病风险间存在剂量反应关系。 Abstract:Objective To analyze the incidence of stroke in the population of Jinchang Cohort, and explore the relationship of diabetes and fasting plasma glucose (FPG) with the risk of stroke, to provide a scientific basis for the control and prevention of stroke. Methods The prospective cohort study was used to analyze the relationship of diabetes and blood glucose levels with the risk of stroke in Jinchang Cohort. The restriction spline method was used to analyze the dose-response relationship between FPG and the risk of stroke. Results A total of 32 736 people were included in this study. After an average follow-up of 2.2 years, the cumulative incidence of stroke was 8.77‰, among which the incidence of stroke in the diabetic group was 23.38‰, which was 6.67‰ higher than that in the control group. After adjusting for confounding factors, the risk of stroke in diabetes group and pre-diabetes group was 2.257 times that of the control group (HR=2.257, 95% CI: 1.658-3.072, P < 0.001) and 1.396 times (HR=1.396, 95% CI: 1.039-1.877, P=0.027), respectively. After controlling for confounding factors, compared with FPG < 5.6 mmol/L, the risk of stroke in the FPG≥5.6 mmol/L group and FPG≥7.0 mmol/L group increased by 48% (HR=1.481, 95% CI: 1.040-2.108) and 49% (HR=1.493, 95% CI: 1.044-2.136) among the total population, respectively; when FPG ≥ 7.0 mmol/L, the risk of stroke in men and women was 1.614 times (HR=1.614, 95% CI: 1.068-2.438) and 2.742 times (HR=2.742, 95% CI: 1.355-5.547) then that of the control group, respectively. There was a nonlinear dose-response relationship between FPG and the risk of stroke among the total population and women. In addition, there was a linear dose-response relationship between FPG and the risk of stroke among men. Conclusion Diabetes is an independent risk factor for stroke, and there is a dose-response relationship between PFG and the risk of stroke. -
Key words:
- Jinchang Cohort /
- Stroke /
- Diabetes /
- Dose-response relationship /
- Prospective study
-
表 1 2011年6月22日―2013年12月30日金昌队列基线情况[n(%)]
Table 1. Baseline situation of Jinchang Cohort from June 22, 2011 to December 30, 2013 [n(%)]
变量 脑卒中组(n=287) 非脑卒中组(n=32 449) t/χ2值 P值 年龄[(x±s),岁] 62.67±9.64 45.96±12.57 22.465 < 0.001 性别 13.017 < 0.001 男 204(71.08) 19 675(60.63) 女 83(28.92) 12 774(39.37) 家庭人均月收入(元) 13.981 < 0.001 < 1 000 8(2.79) 1470(4.53) 1 000~<2 000 165(57.49) 15 126(46.62) ≥2 000 114(39.72) 15 852(48.85) 吸烟 21.999 < 0.001 否 119(41.46) 17 942(55.29) 是 168(58.54) 14 507(44.71) 饮酒 3.082 0.079 否 209(72.82) 25 048(77.19) 是 78(27.18) 7 401(22.81) 脑卒中家族史 0.630 0.427 无 269(93.73) 28 768(94.78) 有 18(6.27) 1 573(5.22) 糖尿病 78.484 < 0.001 无 167(58.19) 24 896(76.72) IFG 64(22.30) 5 214(16.07) 糖尿病 56(9.51) 2 339(7.21) 表 2 糖尿病对脑卒中的发病风险分析
Table 2. Analysis of diabetes on the risk of stroke
组别 N a n b Inc c值(‰) 随访时间(人年) 发病密度(/10万人年) 模型1 d 模型2 e HR(95% CI)值 P值 HR(95% CI)值 P值 对照组 25 063 167 6.67 55 139 30.29 1.000 1.000 IFG组 5 278 64 12.13 11 611 55.12 1.452(1.088~1.938) 0.011 1.396(1.039~1.877) 0.027 糖尿病 2 395 56 23.38 5 269 1 062.28 2.289(1.690~3.101) < 0.001 2.257(1.658~3.072) < 0.001 注:a为总人数; b为脑卒中新发病例数; c为脑卒中发病率; d采用单因素分析; e为调整年龄、性别、收入、吸烟、饮酒、SBP、DBP、脑卒中家族史、体育锻炼后的模型。 表 3 总人群基线FPG与脑卒中发病风险分析
Table 3. Analysis of baseline FPG on the risk of stroke in the total population
基线FPG值(mmol/L) N a n b Inc(%)值 模型1 模型2 HR(95% CI)值 P值 HR(95% CI)值 P值 < 5.6 25 036 171 0.68 1.000 1.000 5.6~ < 6.1 3 153 39 1.24 1.503(1.061~2.129) 0.022 1.481(1.040~2.108) 0.030 6.1~ < 7.0 2 658 39 1.47 1.551(1.095~2.197) 0.014 1.493(1.044~2.136) 0.028 ≥7.0 1 889 38 2.01 1.984(1.396~2.822) < 0.001 1.939(1.358~2.768) < 0.001 注:a为总人数; b为脑卒中新发病例数。 表 4 不同性别人群基线FPG与脑卒中发病风险分析
Table 4. Analysis of baseline FPG on the risk of stroke among different gender population
基线FPG值(mmol/L) 男性 女性 N a n b Inc(%)值 模型1 模型2 N a n b Inc(%)值 模型1 c 模型2 d HR(95% CI)值 HR(95% CI)值 HR(95% CI)值 HR(95% CI)值 < 5.6 14 540 114 0.78 1.000 1.000 10 496 57 0.54 1.000 1.000 5.6~ < 6.1 2 107 29 1.38 1.307(0.869~1.967) 1.370(0.903~2.077) 1 046 10 0.96 1.629(0.832~3.189) 1.597(0.815~3.129) 6.1~ < 7.0 1 853 32 1.73 1.421(0.959~2.106) 1.445(0.962~2.170) 805 7 0.87 1.333(0.608~2.923) 1.283(0.585~2.815) ≥7.0 1 379 29 2.10 1.515(1.007~2.280) 1.614(1.068~2.438) 510 9 1.76 2.825(1.397~5.711) 2.742(1.355~5.547) P趋势 < 0.001 0.015 0.008 0.003 0.006 0.008 注:a为总人数; b为脑卒中新发病例数; c采用单因素分析; d为调整年龄、收入、吸烟、饮酒、SBP、DBP、脑卒中家族史、体育锻炼、降糖药物使用情况后的模型。 -
[1] Sina H, Mustary T, Ahmed K, et al. Association between hypertension and the severity of new onset ischemic stroke in diabetic patients[J]. Journal of Dhaka Medical College, 2020, 28(1): 7-10. DOI: 10.3329/jdmc.v28i1.45749. [2] 《中国脑卒中防治报告》编写组. 《中国脑卒中防治报告2019》概要[J]. 中国脑血管病杂志, 2020, 17(5): 272-281. DOI: 10.3969/j.issn.1672-5921.2020.05.008.Report on stroke prevention and treatment in China writing group. Brief report on stroke prevention and treatment in China, 2019[J]. Chin J Cerebrovasc Dis, 2020, 17(5): 272-281. DOI: 10.3969/j.issn.1672-5921.2020.05.008. [3] Lees KR, Walters MR. Acute stroke and diabetes[J]. Cerebrovasc Dis, 2005, 20(1): 9-14. DOI: 10.1159/000088232. [4] Sarwar N, Gao P, Seshasai SR, et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies[J]. Lancet, 2010, 375(9733): 2215-2222. DOI: 10.1016/S0140-6736(10)60484-9. [5] Liu F, Yang X, Li J, et al. Association of fasting glucose levels with incident atherosclerotic cardiovascular disease: an 8-year follow-up study in a Chinese population[J]. J Diabetes, 2017, 9(1): 14-23. DOI: 10.1111/1753-0407.12380. [6] 余成, 王敏珍, 靳亚飞, 等. 家族史和肥胖交互作用对糖尿病前期人群糖尿病发病的影响[J]. 中华疾病控制杂志, 2020, 24(9): 997-1002. DOI: 10.16462/j.cnki.zhjbkz.2020.09.002.Yu C, Wang MZ, Jin YF, et al. Prospective cohort study of the interaction between family history and obesity on the incidence of diabetes in pre-diabetics[J]. Chin J Dis Control Prev, 2020, 24(9): 997-1002. DOI: 10.16462/j.cnki.zhjbkz.2020.09.002. [7] Cai XY, Zhang YL, Li MJ, et al. Association between prediabetes and risk of all cause mortality and cardiovascular disease: updated meta-analysis[J]. BMJ, 2020, 370: m2297. DOI: 10.1136/bmj.m2297. [8] 薛庆. 空腹血糖受损合并多种危险因素与心脑血管疾病的关系[D]. 苏州: 苏州大学, 2018.Xue Q. Clustering of impaired fasting glucose with cardiovascular risk factors and cardio-cerebrovascular disease[D]. Suzhou: Suzhou University, 2018. [9] Kokubo Y, Okamura T, Watanabe M, et al. The combined impact of blood pressure category and glucose abnormality on the incidence of cardiovascular diseases in a Japanese urban cohort: the suita study[J]. Hypertens Res, 2010, 33(12): 1238-1243. DOI: 10.1038/hr.2010.174. [10] Bai YN, Yang AM, Pu HQ, et al. Cohort profile: the China metal-exposed workers cohort study (Jinchang cohort)[J]. Int J Epidemiol, 2017, 46(4): 1095-1096. DOI: 10.1093/ije/dyw223. [11] Association AD. Report of the expert committee on the diagnosis and classification of diabetes mellitus[J]. Diabetes Care, 2003, 26(1): 5-20. DOI: 10.2337/diacare.20.7.1183. [12] 王新德. 各类脑血管疾病诊断要点[J]. 中华神经科杂志, 1996, 29(6): 60-61. https://www.cnki.com.cn/Article/CJFDTOTAL-SYLC201307036.htmWang XD. Diagnosis points of various cerebrovascular diseases[J]. Chin J Neurol, 1996, 29(6): 60-61. https://www.cnki.com.cn/Article/CJFDTOTAL-SYLC201307036.htm [13] Almdal T, Scharling H, Jensen JS, et al. The independent effect of type 2 diabetes mellitus on ischemic heart disease, stroke, and death[J]. Archives of Internal Medicine, 2004, 164(13): 1422-1426. DOI: 10.1001/archinte.164.13.1422. [14] 高娜, 赵铁耘, 李秀钧. 糖尿病是卒中的独立危险因素[J]. 中国卒中杂志, 2007, 7(7): 594-596. DOI: 10.3969/j.issn.1673-5765.2007.07.012.Gao N, Zhao TY, Li XJ. Diabetes is an independent risk factor for stroke[J]. Chin J Stroke, 2007, 7(7): 594-596. DOI: 10.3969/j.issn.1673-5765.2007.07.012. [15] 朱凌云, 孙侃, 李晓军. 糖尿病合并脑梗死的临床特点与机制研究进展[J]. 医学综述, 2008, 14(7): 1075-1077. DOI: 10.3969/j.issn.1006-2084.2008.07.046.Zhu LY, Sun K, Li XJ. Study progress about clinical characteristics and mechanism of cerebral infarction with diabetes[J]. Medical Recapitulate, 2008, 14(7): 1075-1077. DOI: 10.3969/j.issn.1006-2084.2008.07.046. [16] Mijajlović MD, Aleksić VM, Šternić NM, et al. Role of prediabetes in stroke[J]. Neuropsychiatr Dis Treat, 2017, (13): 259-267. DOI: 10.2147/NDT.S128807. [17] Tanne D, Koren-Morag N, Goldbourt U. Fasting plasma glucose and risk of incident ischemic stroke or transient ischemic attacks: a prospective cohort study[J]. Stroke, 2004, 35(10): 2351-2355. DOI: 10.1161/01.STR.0000140738.94047.55. [18] 吕晓, 黄城意. 空腹血糖受损切点下调与动脉粥样硬化的关系[J]. 现代实用医学, 2014, 26(4): 415-417. DOI: 10.3969/j.issn.1671-0800.2014.04.024.Lu X, Huang CY. The relationship between down-regulation of impaired fasting blood glucose cut-off point and atherosclerosis[J]. Modern Practical Medicine, 2014, 26(4): 415-417. DOI: 10.3969/j.issn.1671-0800.2014.04.024. [19] Lehto S, Rönnemaa T, Pyörälä K, et al. Predictors of stroke in middle-aged patients with non-insulin-dependent diabetes[J]. Stroke, 1996, 27(1): 63-68. DOI: 10.1161/01.STR.27.1.63. [20] Peters SA, Huxley RR, Woodward M. Diabetes as a risk factor for stroke in women compared with men: a systematic review and meta-analysis of 64 cohorts, including 775, 385 individuals and 12, 539 strokes[J]. Lancet, 2014, 383(9933): 1973-1980. DOI: 10.1016/S0140-6736(14)60040-4. [21] 李修英, 刘素贞, 吴清清. 18~59岁2型糖尿病患者饮食行为依从性及影响因素研究[J]. 预防医学, 2020, 32(7): 709-711, 714. DOI: 10.19485/j.cnki.issn2096-5087.2020.07.015.Li XY, Liu SZ, Wu QQ. Study on dietary behavior compliance and influencing factors of patients with type 2 diabetes aged 18-59[J]. Prev Med, 2020, 32(7): 709-711, 714. DOI: 10.19485/j.cnki.issn2096-5087.2020.07.015. -





 下载:
下载: