Impacts of ambient particles of differential sizes and sourceson arrhythmias in adults
-
摘要:
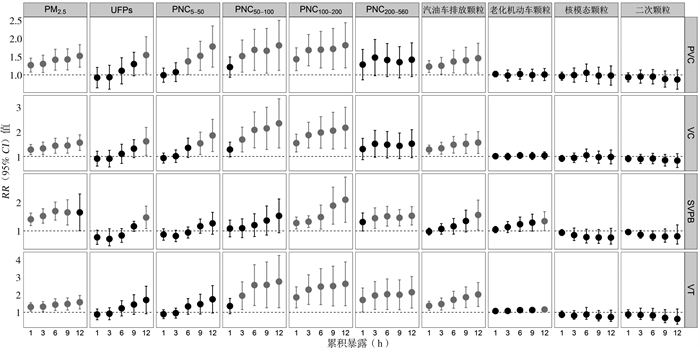
目的 评估不同粒径和大气颗粒物对成年人心律失常的影响。 方法 对73名健康成年人于2014年11月-2016年1月进行4次临床调查,采用24 h动态心电图监测仪记录心律失常逐时发生次数;测定血清中炎性标志物可溶性白介素-1受体拮抗剂(soluble IL-1 receptor antagonist, sIL-1RA)和巨噬细胞炎性蛋白-1β(macrophage inflammatory protein-1β, MIP-1β)水平;监测同期细颗粒物(fine particles matter, PM2.5)、空气动力学直径5.6~560.0 nm不同粒径段颗粒物浓度,以及开展不同粒径尺度颗粒物的源解析。利用广义估计方程模型分析大气颗粒物对心律失常的影响。 结果 累积暴露1 d的超细颗粒物与室性期前收缩(premature ventricular contraction, PVC)、成对室性早搏(ventricular couplets, VC)、室上性期前收缩(supraventricular premature beat, SVPB)、室性心动过速(ventricular tachycardia, VT)的发生存在统计学意义(均有P < 0.05);超细颗粒物每升高IQR浓度的RR值分别为1.89(95% CI: 1.27~2.51)、2.23(95% CI: 1.45~3.00)、1.44(95% CI: 1.12~1.77)和2.63(95% CI: 1.42~3.83)。汽油车排放、老化机动车来源的颗粒物与心律失常发生也呈正相关。分层分析显示,颗粒物致心律失常效应在可溶性白介素-1受体拮抗剂和巨噬细胞炎性蛋白-1β水平高的研究对象中更强。 结论 大气颗粒物特别是其中的交通相关来源的颗粒物可增加成年人发生心律失常的风险,且在全身炎症水平较高者中效应更明显。 Abstract:Objective To assess the impacts of ambient particles of differential sizes and sources on arrhythmias in adults. Methods A total of 73 healthy adults underwent 4 repeated clinical visits between November 2014 and January 2016. At each visit, 24h-ambulatory electrocardiograms were performed to record hourly arrhythmia episodes; And serum inflammatory biomarkers, including soluble IL-1 receptor antagonist and macrophage inflammatory protein-1β were also measured. Concentrations of ambient fine particles and particles in size fractions of 5.6-560.0 nm were monitored throughout the study period. Generalized estimating equation models were conducted to evaluate the impacts of ambient particles on arrhythmias. Results Episodes of premature ventricular contraction, ventricular couplets, supraventricular premature beat, and ventricular tachycardia were positively associated with interquartile range increases in ultrafine particles at prior 1-day moving average of exposure (P < 0.05), with relative risks of 1.89 (95% CI: 1.27-2.51), 2.23 (95% CI: 1.45-3.00), 1.44 (95% CI: 1.12-1.77), and 2.63 (95% CI: 1.42-3.83), respectively. Particles originated from secondary aerosols and aged vehicle emissions were also associated with arrhythmia episodes. Stratified analyses showed stronger associations in participants with higher levels of soluble IL-1 receptor antagonist and macrophage inflammatory protein-1β. Conclusions Ambient particles, especially particles from traffic emission were capable of increasing risks of arrhythmia episodes in adults, and participants with higher levels of systemic inflammation were prone to the proarrhythmic effects of particles. -
Key words:
- Ambient particle /
- Ultrafine particle /
- Arrhythmia /
- Source apportionment
-
表 1 研究期间大气颗粒物和气象因素分布特征
Table 1. Descriptive characteristics of ambient particles and meteorological factors during the study period
变量 M(P25, P75) IQR PM2.5(μg/m3) 50.2(22.7, 86.6) 63.9 UFPs(个/cm3) 19 083(14 972, 23 604) 8 632 5.6~560.0 nm不同粒径段的颗粒物 PNC5-50(个/cm3) 14 140(10 955, 17 331) 6 376 PNC50-100(个/cm3) 3 997(2 825, 6 546) 3 721 PNC100-200(个/cm3) 1 638(810, 2 858) 2 048 PNC200-560(个/cm3) 268(84, 642) 558 5.6~560.0 nm不同粒径段的颗粒物源解析 汽油车排放颗粒(个/cm3) 4 253(1 965, 8 816) 6 851 老化机动车颗粒(个/cm3) 392(115, 1 432) 1 317 二次颗粒(个/cm3) 2 004(560, 4 281) 3 721 核模态颗粒(个/cm3) 10 381(7 729, 13 409) 5 680 其他(个/cm3) 697(118, 2 286) 2 168 气象参数 温度(℃) 6.9(0.7, 20.7) 20.0 相对湿度(%) 27.9(21.0, 44.6) 23.6 表 2 大气颗粒物每升高IQR浓度时以研究对象炎症指标水平中位数分层的心律失常RR值及95% CI值
Table 2. Arrhythmia episodes (RR and 95% CI) associated with per IQR increase in ambient particles stratified by median levels of inflammatory indicators of study participants
指标 污染物 累积暴露(d) RR (95% CI)值 P值 RR (95% CI) 值 P值 sIL-1RA < M sIL-1RA M MIP-1β < M MIP-1β M PVC UFPs 1 1.20 (0.96~1.44) 2.21 (1.45~2.98) 0.012 1.15 (0.75~1.55) 2.49 (1.30~3.69) 0.053 2 1.24 (0.81~1.67) 4.37 (2.12~6.61) 0.003 1.95 (0.86~3.05) 4.51 (1.87~7.14) 0.174 5 1.03 (0.53~1.53) 5.54 (1.75~9.34) 0.013 1.30 (0.40~2.20) 5.42 (1.65~9.19) 0.095 汽油车排放颗粒物 1 0.93 (0.61~1.25) 1.45 (0.93~1.96) 0.155 0.86 (0.52~1.19) 2.09 (1.36~2.83) 0.008 2 0.92 (0.44~1.40) 4.97 (1.69~8.24) 0.011 0.91 (0.38~1.43) 6.31 (2.98~9.64) < 0.001 5 1.25 (0.34~2.16) 2.03 (0.80~3.27) 0.551 0.30 (0.09~1.04) 2.78 (1.32~4.24) 0.003 VC UFPs 1 1.01 (0.98~1.04) 2.07 (1.44~2.71) < 0.001 1.15 (0.75~1.55) 1.75 (1.08~2.42) 0.202 2 1.01 (0.97~1.05) 3.83 (2.06~5.59) < 0.001 1.95 (0.86~3.05) 2.49 (1.30~7.14) 0.648 5 1.03 (0.99~1.07) 5.94 (1.89~9.98) 0.003 1.30 (0.40~2.20) 4.23 (1.65~6.81) 0.124 汽油车排放颗粒物 1 1.00 (0.57~1.44) 1.48 (0.93~2.04) 0.300 0.84 (0.44~1.24) 2.28 (1.38~3.18) 0.017 2 0.77 (0.33~1.22) 4.65 (1.49~7.82) 0.014 0.83 (0.30~1.36) 6.38 (2.80~9.96) 0.002 5 1.68 (0.39~2.97) 2.07 (0.78~3.36) 0.814 0.32 (0.08~1.27) 2.67 (1.21~4.14) 0.009 注:sIL-1RA的M值为53.8 pg/mL;MIP-1β的M值为333.3 pg/mL。 -
[1] Bei Y, Shi C, Zhang Z, et al. Advance for cardiovascular health in China[J]. J Cardiovasc Transl Res, 2019, 12(3): 165-170. DOI: 10.1007/s12265-018-9852-7. [2] Brook RD, Rajagopalan S, Pope CA, et al. Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association[J]. Circulation, 2010, 121(21): 2331-2378. DOI: 10.1161/CIR.0b013e3181dbece1. [3] Zhang S, Lu W, Wei Z, et al. Air pollution and cardiac arrhythmias: from epidemiological and clinical evidences to cellular electrophysiological mechanisms[J]. Front Cardiovasc Med, 2021, 8: 736151. DOI: 10.3389/fcvm.2021.736151. [4] Stone V, Miller MR, Clift MJD, et al. Nanomaterials versus ambient ultrafine particles: an opportunity to exchange toxicology knowledge[J]. Environ Health Perspect, 2017, 125(10): 106002. DOI: 10.1289/EHP424. [5] Berger A, Zareba W, Schneider A, et al. Runs of ventricular and supraventricular tachycardia triggered by air pollution in patients with coronary heart disease[J]. J Occup Environ Med, 2006, 48(11): 1149-1158. DOI: 10.1097/01.jom.0000245921.15916.03. [6] Langrish JP, Watts SJ, Hunter AJ, et al. Controlled exposures to air pollutants and risk of cardiac arrhythmia[J]. Environ Health Perspect, 2014, 122(7): 747-753. DOI: 10.1289/ehp.1307337. [7] Li J, Zhou C, Xu H, et al. Ambient air pollution is associated with HDL (high-density lipoprotein) dysfunction in healthy adults[J]. Arterioscler Thromb Vasc Biol, 2019, 39(3): 513-522. DOI: 10.1161/ATVBAHA.118.311749. [8] Hennig F, Quass, Hellack B, et al. Ultrafine and fine particle number and surface area concentrations and daily cause-specific mortality in the Ruhr Area, Germany, 2009-2014[J]. Environ Health Perspect, 2018, 126(2): 027008. DOI: 10.1289/EHP2054. [9] Xu H, Wang T, Liu S, et al. Extreme levels of air pollution associated with changes in biomarkers of atherosclerotic plaque vulnerability and thrombogenicity in healthy adults[J]. Circ Res, 2019, 124(5): e30-e43. DOI: 10.1161/CIRCRESAHA.118.313948. [10] Xu H, Chen J, Zhao Q, et al. Ambient air pollution is associated with cardiac repolarization abnormalities in healthy adults[J]. Environ Res, 2019, 171: 239-246. DOI: 10.1016/j.envres.2019.01.023. [11] Dockery DW, Luttmann-Gibson H, Rich DQ, et al. Association of air pollution with increased incidence of ventricular tachyarrhythmias recorded by implanted cardioverter defibrillators[J]. Environ Health Perspect, 2005, 113(6): 670-674. DOI: 10.1289/ehp.7767. [12] Zhao A, Chen R, Kuang X, et al. Ambient air pollution and daily outpatient visits for cardiac arrhythmia in Shanghai, China[J]. J Epidemiol, 2014, 24(4): 321-326. DOI: 10.2188/jea.je20140030. [13] Wang M, Chen J, Zhang Z, et al. Associations between air pollution and outpatient visits for arrhythmia in Hangzhou, China[J]. BMC Public Health, 2020, 20(1): 1524. DOI: 10.1186/s12889-020-09628-y. [14] Bartell SM, Longhurst J, Tjoa T, et al. Particulate air pollution, ambulatory heart rate variability, and cardiac arrhythmia in retirement community residents with coronary artery disease[J]. Environ Health Perspect, 2013, 121(10): 1135-1141. DOI: 10.1289/ehp.1205914. [15] Miller MR, Raftis JB, Langrish JP, et al. Inhaled nanoparticles a accumulate at sites of vascular disease[J]. ACS Nano, 2017, 11(5): 4542-4552. DOI: 10.1021/acsnano.6b08551. [16] Mills NL, Finlayson AE, Gonzalez MC, et al. Diesel exhaust inhalation does not affect heart rhythm or heart rate variability[J]. Heart, 2011, 97(7): 544-550. DOI: 10.1136/hrt.2010.199042. [17] Arend WP, Malyak M, Guthridge CJ. Interleukin-1 receptor antagonist: role in biology[J]. Annu Rev Immunol, 1998, 16: 27-55. DOI: 10.1146/annurev.immunol.16.1.27. [18] Huang W, Zhu T, Pan X, et al. Air pollution and autonomic and vascular dysfunction in patients with cardiovascular disease: interactions of systemic inflammation, overweight, and gender[J]. Am J Epidemiol, 2012, 176(2): 117-126. DOI: 10.1093/aje/kwr511. -





 下载:
下载: