Relationship between advanced sleep phase syndrome and type 2 diabetes mellitus based on the propensity score method
-
摘要:
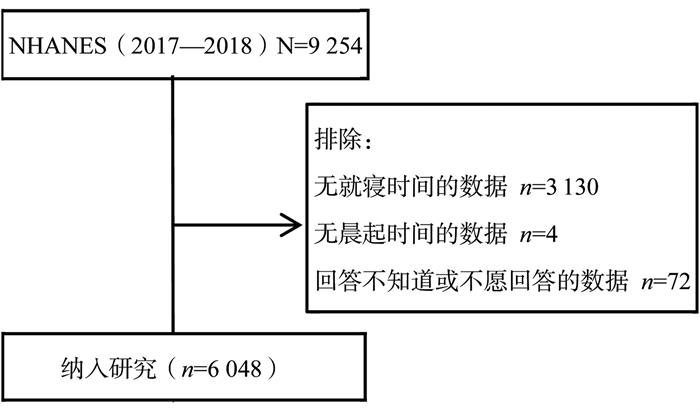
目的 探讨睡眠时相提前综合征(advanced sleep phase syndrome, ASPS)和2型糖尿病(type 2 diabetes mellitus, T2DM)间的关联性,为深入理解睡眠的健康效应及预防和干预T2DM提供理论依据。 方法 本研究数据来源于美国国家健康和营养调查(National Health and Nutrition Examination Survey, NHANES)(2017-2018年)数据库。ASPS由工作日的就寝时间和晨起时间定义。T2DM根据服用降糖药物来定义。使用基于倾向性评分的逆概率加权法(inverse probability treatment weight, IPTW)和重叠加权法(overlap weights, OW)尽可能地控制潜在混杂变量后,分析ASPS和T2DM的关联性。 结果 共有6 048名研究对象被纳入研究,其中759人患有T2DM,411人被诊断为ASPS,分别占12.5%、6.8%。T2DM在ASPS组中的患病率比非ASPS组高(20.0% vs. 12.0%, t=21.295, P < 0.001)。IPTW控制潜在混杂后,分析显示ASPS组患T2DM的风险是非ASPS组的1.540倍(OR=1.540, 95% CI: 1.184~2.002, P=0.001);OW进一步完全均衡协变量后,分析显示二者差异有统计学意义(OR=1.362, 95% CI: 1.078~1.722, P=0.001)。 结论 ASPS是T2DM独立风险因素,提示睡眠问题的管理在T2DM的防制中具有重要意义。 Abstract:Objective This study aimed to analyze the correlation between advanced sleep phase syndrome (ASPS) and type 2 diabetes mellitus (T2DM), to better understand the health effects of sleep and provide a theoretical basis for prevention and intervention of T2DM. Methods The data for this study were obtained from the National Health and Nutrition Examination Survey (NHANES) (2017-2018) database. ASPS was defined by bedtime and morning rise time on weekdays. T2DM was defined as taking antidiabetic drugs. Associations between ASPS and T2DM were analyzed using the propensity score-based inverse probability treatment weights (IPTW) and overlap weights (OW) to control for potential confounding variables as much as possible. Results A total of 6 048 participants were included in the study, of whom 759 had T2DM and 411 were diagnosed with ASPS, accounting for 12.5% and 6.8%, respectively. The prevalence of T2DM was higher in the ASPS group than in the non-ASPS group (20.0% vs. 12.0%, t=21.295, P < 0.001). After controlling for potential confounding by IPTW, the analysis showed that the ASPS group had a 1.540-fold higher risk of developing T2DM than the non-ASPS group (OR=1.540, 95% CI: 1.184-2.002, P=0.001). After further fully balancing the covariates, OW analysis showed the significance of the two still existed (OR=1.362, 95% CI: 1.078-1.722, P=0.001). Conclusions ASPS is an independent risk factor for T2DM, suggesting that the management of sleep problems is of great significance in the prevention and treatment of T2DM. -
表 1 研究人群基本特征[n(%)]
Table 1. Characteristics of the study population [n(%)]
基本特征 总人数(N=6 048) ASPS(n=411) 非ASPS(n=5 637) t/χ2值 P值 睡眠时长(x±s, h) 7.68±1.61 7.71±0.94 7.67±1.65 0.505 0.613 糖尿病史 0.649 0.421 是 1 081(17.9) 80(19.5) 1 001(17.8) 否 4 967(82.1) 331(80.5) 4 636(82.2) 抑郁史 0.353 0.552 是 1 269(21.0) 81(19.7) 1 188(21.1) 否 4 779(79.0) 330(80.3) 4 449(78.9) 年龄(x±s, 岁) 48.14±19.69 52.06±16.34 47.86±19.89 4.185 < 0.001 性别 3.404 0.065 男 2 935(48.5) 218(53.0) 2 717(48.2) 女 3 113(51.5) 193(47.0) 2 920(51.8) 种族 27.972 < 0.001 墨西哥裔美国人 838(13.9) 86(20.9) 752(13.3) 非西班牙裔白人 2 093(34.6) 126(30.7) 1 967(34.9) 非西班牙裔黑人 1 914(31.6) 143(34.8) 1 771(31.4) 其他 1 203(19.9) 56(13.6) 1 147(20.3) 受教育水平 44.634 < 0.001 高中或以下 2 662(44.0) 229(55.7) 2 433(43.2) 大学 2 044(33.8) 142(34.5) 1 902(33.7) 大学毕业及以上 1 342(22.2) 40(9.7) 1 302(23.1) 婚姻状况 2.627 0.269 已婚 2 706(44.7) 195(47.4) 2 511(44.5) 与伴侣同住 742(12.3) 41(10.0) 701(12.4) 单身 2 600(43.0) 175(42.6) 2 425(43.0) 家庭收入与贫困比例 0.775 0.679 < 1.3 2 372(39.2) 166(40.4) 2 206(39.1) 1.3~3.5 2 139(35.4) 148(36.0) 1 991(35.3) >3.5 1 537(25.4) 97(23.6) 1 440(25.5) BMI(kg/m2) 20.510 < 0.001 < 18.5 541(8.9) 41(10.0) 500(8.9) 18.5~ < 24.0 1 174(19.4) 55(13.4) 1 119(19.9) 24.0~ < 28.0 1 414(23.4) 78(19.0) 1 336(23.7) ≥28.0 2 919(48.3) 237(57.7) 2 682(47.6) 饮酒状况 2.603 0.107 ≤1杯/d 3 894(64.4) 249(60.6) 3 645(64.7) >1杯/d 2 154(35.6) 162(39.4) 1 992(35.3) 吸烟状况 6.171 0.046 每天 920(15.2) 74(18.0) 846(15.0) 偶尔 2 711(44.8) 195(47.4) 2 516(44.6) 不吸 2 417(40.0) 142(34.5) 2 275(40.4) 高血压史 17.656 < 0.001 是 2 095(34.6) 182(44.3) 1 913(33.9) 否 3 953(65.4) 229(55.7) 3 724(66.1) 健康状况 33.404 < 0.001 非常好 1 985(32.8) 83(20.2) 1 902(33.7) 好或一般 3 904(64.6) 319(77.6) 3 585(63.6) 差 159(2.6) 9(2.2) 150(2.7) 身体活动度 1.178 0.555 剧烈 1 480(24.5) 93(22.6) 1 387(24.6) 适度 1 477(24.4) 98(23.8) 1 379(24.5) 无 3 091(51.1) 220(53.5) 2 871(50.9) T2DM 21.295 < 0.001 否 5 289(87.5) 329(80.0) 4 960(88.0) 是 759(12.5) 82(20.0) 677(12.0) 表 2 ASPS与T2DM的相关性分析
Table 2. Analyses of the association between ASPS and T2DM
模型 OR (95% CI)值 χ2值 P值 单因素模型 1.826 (1.415~2.356) 4.630 < 0.001 模型1 1.619 (1.208~2.169) 3.222 0.001 模型2 1.540 (1.184~2.002) 3.221 0.001 模型3 1.362 (1.078~1.722) 2.586 0.001 注:单因素模型:未校正混杂因素;模型1、2、3:校正年龄、性别、种族、教育水平等在内的所有协变量。 -
[1] Weng Z, Ou W, Huang J, et al. Circadian misalignment rather than sleep duration is associated with MAFLD: a population-based propensity score-matched study[J]. Nat Sci Sleep, 2021, 13: 103-111. DOI: 10.2147/NSS.S290465. [2] 韩芳. 昼夜节律性睡眠障碍[J]. 生命科学, 2015, 27(11): 1448-1454. DOI: 10.13376/j.cbls/2015200.Han F. Circadian rhythm sleep disorder[J]. Life Science, 2015, 27(11): 1448-1454. DOI: 10.13376/j.cbls/2015200. [3] Sateia MJ. International classification of sleep disorders-third edition: highlights and modifications[J]. Chest, 2014, 146(5): 1387-1394. DOI: 10.1378/chest.14-0970. [4] Ando K, Kripke DF, Ancoli-Israel S. Delayed and advanced sleep phase symptoms[J]. Isr J Psychiatry Relat Sci, 2002, 39(1): 11-18. DOI: 10.1017/S1041610203008688. [5] Meng Q, Qi X, Fu Y, et al. Flavonoids extracted from mulberry (Morus alba L. ) leaf improve skeletal muscle mitochondrial function by activating AMPK in type 2 diabetes[J]. J Ethnopharmacol, 2020, 248: 112326. DOI: 10.1016/j.jep.2019.112326. [6] Wang L, Gao P, Zhang M, et al. Prevalence and ethnic pattern of diabetes and prediabetes in China in 2013[J]. JAMA, 2017, 317(24): 2515-2523. DOI: 10.1001/jama.2017.7596. [7] 王文华. 睡眠障碍和2型糖尿病的关系: meta分析和孟德尔随机化研究[D]. 郑州: 郑州大学, 2018.Wang WH. The relationship between sleep disturbance and type 2 diabetes: meta-analysis and Mendelian randomization study[D]. Zhengzhou: Zhengzhou University, 2018. [8] Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects[J]. Biometrika, 1983, 20(1): 41-55. DOI: 10.1093/biomet/70.1.41. [9] Cappuccio FP, D'Elia L, Strazzullo P, et al. Quantity and quality of sleep and incidence of type 2 diabetes: a systematic review and meta-analysis[J]. Diabetes Care, 2010, 33(2): 414-420. DOI: 10.2337/dc09-1124. [10] Rod NH, Vahtera J, Westerlund H, et al. Sleep disturbances and cause-specific mortality: results from the GAZEL cohort study[J]. Am J Epidemiol, 2011, 173(3): 300-309. DOI: 10.1093/aje/kwq371. [11] Austin PC, Stuart EA. Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies[J]. Stat Med, 2015, 34(28): 3661-3679. DOI: 10.1002/sim.6607. [12] Johnson CL, Paulose-Ram R, Ogden CL, et al. National health and nutrition examination survey: analytic guidelines, 1999-2010[J]. Vital Health Stat 2, 2013, (161): 1-24. [13] DeShields SC, Cunningham TD. Comparison of osteoporosis in US adults with type 1 and type 2 diabetes mellitus[J]. J Endocrinol Invest, 2018, 41(9): 1051-1060. DOI: 10.1007/s40618-018-0828x. [14] Lee M, Lee S. Double robustness without weighting[J]. Stat Probab Lett, 2019, 146: 175-180. DOI: 10.1016/j.spl.2018.11.017. [15] Li F, Morgan KL, Zaslavsky AM. Balancing covariates via propensity score weighting[J]. J Am Stat Assoc, 2016, 113: 390-400. DOI: 10.1080/01621459.2016.1260466. [16] 秦宇辰, 郭威, 阮一鸣, 等. 重叠加权法在医学研究混杂因素控制中的应用[J]. 中国卫生统计, 2020, 37(3): 363-366.Qin YC, Guo W, Ruan YM, et al. Application of overlapping weighting method in the control of confounding factors in medical research[J]. Chin J Health Statistics, 2020, 37(3): 363-366. [17] Patke A, Young MW, Axelrod S. Molecular mechanisms and physiological importance of circadian rhythms[J]. Nat Rev Mol Cell Biol, 2020, 21(2): 67-84. DOI: 10.1038/s41580-019-0179-2. [18] Toh KL, Jones CR, He Y, et al. An hPer2 phosphorylation site mutation in familial advanced sleep phase syndrome[J]. Science, 2001, 291(5506): 1040-1043. DOI: 10.1126/science.1057499. [19] Takahashi JS. Transcriptional architecture of the mammalian circadian clock[J]. Nat Rev Genet, 2017, 18(3): 164-179. DOI: 10.1038/nrg.2016.150. [20] 陈筵明, 龚维坤, 孙英芬, 等. 昼夜节律紊乱与2型糖尿病关系的研究进展[J]. 中国细胞生物学学报, 2020, 42(9): 1684-1693. DOI: 10.11844/cjcb.2020.09.0023.Chen YM, Gong WK, Sun YF, et al. Research progress on the relationship between circadian rhythm disturbance and type 2 diabetes mellitus[J]. Chinese Journal of Cell Biology, 2020, 42(9): 1684-1693. DOI: 10.11844/cjcb.2020.09.0023. -





 下载:
下载: