The analysis of Human Papillomavirus infection and subtype distribution in 8 744 females in Anhui Province
-
摘要:
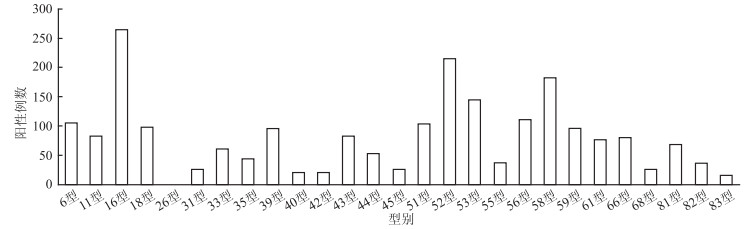
目的 探讨安徽地区女性人乳头瘤病毒(Human Papillomavirus,HPV)分子流行病学现况,为HPV疫苗的推广使用提供参考依据。 方法 采用流式荧光杂交法检测安徽地区8 744例送检女性标本HPV亚型感染情况。 结果 高危型别和低危型别的感染率分别为16.10%和6.38%;HPV单一和多重感染率分别为13.85%和5.58%;HPV16型感染率最高,其次为52型和58型;皖南、皖中、皖北HPV感染率差异有统计学意义(χ2=13.790,P=0.008),皖北高危51型和56型感染率高于其他两个地区,差异有统计学意义(χ2=17.323,P < 0.001;χ2=9.643,P=0.008);10~岁年龄组感染率最高(37.50%),其次是20~岁年龄组(23.19%)和≥ 60岁年龄组(22.16%),各年龄组感染率差异有统计学意义(χ2=61.855,P < 0.001);不同年份HPV亚型感染率差异有统计学意义(χ2=59.479,P < 0.001),2015年份感染率最高。 结论 安徽地区HPV感染主要以高危单一型别感染为主,感染率前3的亚型依次是16型、52型和58型;不同地区HPV感染差异均有统计学意义(均有P < 0.05),个别型别有较高的感染率;HPV感染年龄分布总体呈两头高、中间低的分布趋势;不同年份HPV感染率呈逐年下降趋势。 Abstract:Objective To investigate the genotypes of Human Papillomavirus (HPV) infection and distribution characteristics of women in Anhui, and to provide reference for HPV molecular epidemiology research and promotion of vaccine in Anhui. Methods The flowcytometry fluorescence hybridization method were used to eaxm 8 744 samples of women HPV Subtype. Results The high-risk and low-risk infection rate of HPV were 16.10% and 6.38% respectively. The rate of single and multiple subtype were 13.85% and 5.58% respectively. HPV positive detectable rates were higher in HPV16, HPV52 and HPV58, HPV16 was the highest. The defection rate was significantly different among southern, central and northern in Anhui (χ2=13.790, P=0.008). The infection rates of high risk subtype 51 and 56 in northern were higher than those in the other two regions, and the difference was statistically significant (χ2=17.323, P < 0.001; χ2=9.643, P=0.008). Age distribution results showed that the age group with high infection rate was 10-age group (37.50%), 20-age group (23.19%) and ≥ 60 age group (22.16%), and the difference was statistically significant (χ2=61.855, P < 0.001). The infection rates of HPV subtypes in different years were significantly different (χ2=59.479, P < 0.001). The infection rate was the highest in 2015. Conclusions The high risk and single genotypes of infection were dominant in Anhui. HPV positive detectable rates were higher in HPV16, HPV52 and HPV58. There was significant difference in different regions (all P < 0.05) and there were some subtypes with higher infection rates. The age distribution of HPV infection showed a trend of high in youngest and oldest group and low in the middle. The infection rate in different years showed a downward trend year by year. -
Key words:
- Anhui Province /
- HPV genotype /
- Infection rate /
- Distribution
-
表 1 不同地区HPV亚型感染情况[n(%)]
Table 1. Situation of HPV subtype infection in different regions[n(%)]
地区 总感染率 高危 低危 51型 56型 单一 多重 单一 多重 单一 多重 皖北 695(14.70) 287(6.07) 633(13.39) 175(3.70) 282(5.96) 38(0.80) 77(1.63) 82(1.70) 皖中 328(12.86) 137(5.37) 312(12.23) 80(3.14) 130(5.10) 20(0.78) 28(1.10) 27(1.10) 皖南 188(12.84) 64(4.37) 176(12.02) 32(2.19) 80(5.46) 8(0.55) 4(0.27) 12(0.80) χ2值 13.790 11.985 3.482 17.323 9.643 P值 0.008 0.017 0.481 < 0.001 0.008 表 2 不同年龄组HPV亚型感染情况[n(%)]
Table 2. Situation of HPV subtype infection in different age groups[n(%)]
年龄组(岁) 阳性 总感染率 高危 低危 单一 多重 单一 多重 单一 多重 10~ 51(37.50) 30(22.06) 21(15.44) 26(19.12) 18(13.24) 16(11.76) 1(0.74) 20~ 499(23.19) 314(14.59) 185(8.60) 301(13.99) 115(5.34) 158(7.34) 29(1.35) 30~ 448(17.20) 326(12.51) 122(4.68) 308(11.82) 65(2.50) 126(4.84) 17(0.65) 40~ 484(18.07) 377(14.07) 107(3.99) 339(12.65) 61(2.28) 125(4.67) 14(0.52) 50~ 174(17.79) 139(14.21) 35(3.58) 123(12.58) 15(1.53) 55(5.62) 4(0.41) ≥60岁 43(22.16) 25(12.89) 18(9.28) 24(12.37) 13(6.70) 12(6.19) 1(0.52) 合计 1 699(19.43) 1 211(13.84) 488(5.58) 1 121(12.82) 287(3.28) 492(5.63) 66(0.75) χ2值 61.855 109.550 115.788 44.153 P值 < 0.001 < 0.001 < 0.001 < 0.001 表 3 不同年龄组HPV亚型感染分布[n(%)]
Table 3. HPV subtype distribution of different age groups [n(%)]
HPV
亚型总人数
(人)年龄组(岁) 10~ 20~ 30~ 40~ 50~ ≥60 6型 111(1.27) 6(4.41) 46(2.14) 33(1.27) 17(0.63) 6(0.61) 3(1.54) 11型 92(1.05) 9(6.62) 51(2.37) 20(0.77) 5(0.19) 5(0.51) 2(1.03) 16型 299(3.42) 9(6.62) 78(3.62) 66(2.53) 105(3.92) 32(3.27) 9(4.62) 18型 98(1.12) 6(4.41) 32(1.49) 20(0.77) 31(1.16) 6(0.61) 3(1.54) 26型 0(0.00) 0(0.00) 0(0.00) 0(0.00) 0(0.00) 0(0.00) 0(0.00) 31型 28(0.32) 3(2.21) 9(0.42) 8(0.31) 7(0.26) 0(0.00) 1(0.51) 33型 75(0.86) 0(0.00) 19(0.88) 20(0.77) 20(0.75) 8(0.82) 8(4.10) 35型 60(0.69) 4(2.94) 17(0.79) 15(0.58) 15(0.56) 8(0.82) 1(0.51) 39型 108(1.23) 3(2.21) 33(1.53) 33(1.27) 34(1.27) 5(0.51) 0(0.00) 40型 24(0.27) 0(0.00) 11(0.51) 4(0.15) 6(0.22) 3(0.31) 0(0.00) 42型 25(0.29) 0(0.00) 4(0.19) 4(0.15) 12(0.45) 3(0.31) 2(1.03) 43型 87(0.99) 1(0.74) 30(1.39) 27(1.04) 21(0.78) 6(0.61) 2(1.03) 44型 65(0.74) 1(0.74) 13(0.60) 11(0.42) 27(1.01) 11(1.24) 2(1.03) 45型 32(0.37) 0(0.00) 13(0.60) 3(0.12) 14(0.52) 0(0.00) 2(1.03) 51型 109(1.25) 8(5.88) 37(1.72) 29(1.11) 25(0.93) 7(0.72) 3(1.54) 52型 254(2.90) 7(5.15) 73(3.39) 90(3.45) 65(2.43) 13(1.33) 6(3.08) 53型 158(1.81) 8(5.88) 52(2.42) 35(1.34) 35(1.31) 2(2.04) 8(4.10) 55型 38(0.43) 0(0.00) 9(0.42) 10(0.38) 13(0.49) 5(0.51) 1(0.51) 56型 121(1.38) 4(2.94) 46(2.14) 26(1.00) 26(0.97) 17(1.74) 2(1.03) 58型 202(2.31) 3(2.21) 66(3.07) 51(1.96) 56(2.09) 18(1.84) 8(4.10) 59型 108(1.23) 10(7.35) 46(2.14) 21(0.81) 19(0.71) 8(0.82) 3(1.54) 61型 92(1.05) 0(0.00) 20(0.93) 28(1.07) 26(0.97) 17(1.74) 1(0.51) 66型 82(0.94) 3(2.21) 41(1.90) 15(0.58) 15(0.56) 6(0.61) 2(1.03) 68型 26(0.30) 3(2.21) 10(0.46) 9(0.35) 3(0.11) 1(0.10) 0(0.00) 81型 86(0.98) 1(0.74) 24(1.11) 23(0.88) 29(1.08) 8(0.82) 1(0.51) 82型 46(0.53) 3(2.21) 16(0.74) 15(0.58) 6(0.22) 5(0.51) 1(0.51) 83型 16(0.18) 0(0.00) 11(0.51) 2(0.08) 2(0.07) 1(0.10) 0(0.00) 表 4 2015-2017年HPV状况[n(%)]
Table 4. Situation of HPV infection from 2015 to 2017 [n(%)]
年份 阳性 总感染率 高危 低危 单一 多重 单一 多重 单一 多重 2015 258(26.46) 182(18.67) 76(7.79) 160(16.41) 46(4.72) 79(8.10) 13(1.33) 2016 646(21.35) 443(14.64) 203(6.71) 422(13.95) 121(4.00) 189(6.25) 22(0.73) 2017 795(16.76) 586(12.36) 209(4.41) 539(11.36) 120(2.53) 224(4.72) 31(0.65) χ2值 59.479 64.086 46.583 26.166 P值 < 0.001 < 0.001 < 0.001 0.001 -
[1] 魏长慧, 朱继存, 牛媛娜, 等. 2004-2016年中国女性生殖系统恶性肿瘤死亡趋势分析[J]. 中华疾病控制杂志, 2019, 23(5): 506-511. DOI: 10.16462/j.cnki.zhjbkz.2019.05.003.Wei CH, Zhu JC, Niu YN, et al. Analysis of the mortality trend of female reproductive system cancer in China from 2004 to 2016[J]. Chin J Dis Control Prev, 2019, 23(5): 506-511. DOI: 10.16462/j.cnki.zhjbkz.2019.05.003. [2] 王兰芳, 胡双婕, 葛晓伟, 等. HPV不同基因型感染在宫颈病变过程中的研究[J]. 中华疾病控制杂志, 2019, 23(5): 536-544. DOI: 10.16462/j.cnki.zhjbkz.2019.05.009.Wang LF, Hu SJ, Ge XW, et al. Study on genotype-associated HPV infection in cervical lesions[J]. Chin J Dis Control Prev, 2019, 23(5): 536-544. DOI: 10.16462/j.cnki.zhjbkz.2019.05.009. [3] Hausen ZH. Papillomaviruses in human cancers[J]. Proc Assoc Am Physicians, 1999, 111(6): 581-587. [4] Bioscience Division, Los Alamos National Laboratory, the Regents of the University of California. HPV sequence database: PV types and hosts _database online Available at: http://hpv-web.lanl.gov/stdgen/virus/cgi-bin/hpv_organisms.cgi?dbname_hpv Accessed August 23, 2004. [5] Kamnaratne K, Ihalagama H, Rohitha S, et al. Human papillomavrius prevalence and type-distribution in women with cervical lesions: a cross-sectional study in Sri Lanka[J]. BMC Cancel, 2014, 14: 116-122. DOI: 10.1186/1471-2407-14-116. [6] 王薇, 郭健, 陆海涛, 等. 承德地区13120例女性生殖道HPV感染结果分析[J]. 承德医学院学报, 2019, 36(2): 109-111. DOI: 10.15921/j.cnki.cyxb.2019.02.007.Wang W, Guo J, Lu HT, et al. Anaylsis of the results of HPV infection in female genital tract of 13120 cases in Chengde[J]. Journal of Chengde Medical College, 2019, 36(2): 109-111. DOI: 10.15921/j.cnki.cyxb.2019.02.007. [7] Agodi A, Barchitta M, La Rosa N, et al. Human papillomavirus infection: low-risk and high-risk genotypes in women in Catania, Sicily[J]. Int J Gynecol Cancer. 2009, 19(6): 1094-1098. DOI: 10.1111/IGC.0b013e3181a83c9d. [8] Bruni L1, Diaz M, Castellsagué X, et al. Cervical human papillomavirus prevalence in 5 continents: meta-analysis of 1 million women with normal cytological findings[J]. J Infect Dis. 2010, 202(12): 1789-1799. DOI: 10.1086/657321. [9] 李翀, 郑旭. 天津地区4232例妇女宫颈HPV感染基因谱分析[J]. 中国妇幼保健, 2015, 30(10): 1571-1573. DOI: 10.7620/zgfybi.j.issn.1001-4411.2015.10.36.Li C, Zheng X. Genomic analysis of cervical HPV infection in 4232 women in Tianjin[J]. Maternal and Child Health Care of China, 2015, 30(10): 1571-1573. DOI: 10.7620/zgfybi.j.issn.1001-4411.2015.10.36. [10] 李静霞, 刘文利, 刘悦君, 等. 邯郸地区女性人乳头瘤病毒感染基因型分布特点临床分析[J]. 中国妇幼保健, 2017, 32(20): 4926-4928. DOI: 10.7620/zgfybi.j.issn.1001-4411.2017.20.11.Li JX, Liu WL, Liu YJ, et al. Clinical analysis of genotype distribution characteristics of human papillomavirus infection in females in Handan[J]. Maternal and Child Health Care of China, 2017, 32(20): 4926-4928. DOI: 10.7620/zgfybi.j.issn.1001-4411.2017.20.11. [11] 李晓娇, 卢晓佳, 张群峰. 上海市奉贤区人乳头瘤病毒感染状况及型别分布特征[J]. 国际检验医学杂志, 2014, 35(20): 2792-2793. DOI: 10.3969/j.issn.1673-4130.2014.20.032.Li XJ, Lu XJ, Zhang QF. Infection situation and type distribution characteristics of human papillomavirus in Fengxian District of Shanghai[J]. Int J Lab Med, 2014, 35(20): 2792-2793. DOI: 10.3969/j.issn.1673-4130.2014.20.032. [12] 陈静敏, 贾璋林, 符丹雪, 等. HPV亚型与TCT筛查结果的相关性及两者联合在宫颈癌筛查中的应用研究[J]. 国际检验医学杂志, 2017, 38(24): 3482-3485. DOI: 10.3969/j.issn.1673-4130.2017.24.051.Chen JM, Jia ZL, Fu DX, et al. The correlation between HPV subtypes and TCT screening results and the application of the combination of HPV subtypes and TCT in cervical cancer screening[J]. Int J Lab Med, 2014, 35(20): 2792-2793. DOI: 10.3969/j.issn.1673-4130.2017.24.051. [13] 谢珊艳, 任鹏. 宫颈癌发病年轻化的趋势分析与相应对策[J]. 中医药管理杂志, 2018, 26(5): 10-12. DOI: 10.16690/j.cnki.1007-9203.2018.05.005.Xie SY, Ren P. Trend analysis and countermeasures of cervical cancer younger[J]. Journal of Traditional Chinese Medicine Managemen, 2018, 26(5): 10-12. DOI: 10.16690/j.cnki.1007-9203.2018.05.005. [14] 赵丽雅, 庞晓燕, 陈青青, 等. 老年子宫颈高危型HPV感染与子宫颈病变的相关性分析[J]. 中国医科大学学报, 2014, 43(8): 691-693. DOI: 10.3969/j.issn.0258-4646.2014.08.005.Zhao LY, Pang XY, Chen QQ, et al. Correlation analysis between HPV infection and cervical lesions in the elderly females[J]. J China Med Univ, 2014, 43(8): 691-693. DOI: 10.3969/j.issn.0258-4646.2014.08.005. [15] Schuchat A. HPV "Coverage"[J]. N Engl J Med, 2015, 372: 775-776. DOI: 10.1056/NEJMel415742. [16] 王泓沄. 中国长三角地区浸润性宫颈癌和癌前期病变HPV感染型别分布的研究[D]. 杭州: 浙江大学, 2014.Wang HY. Study on the distribution of HPV genotype prevalence in invasive cervical carcinoma and precancerous lesions in Yangtza River Delta Area, China[D]. Hangzhou: Zhejiang University, 2014. [17] 徐元. 新疆地区宫颈病变HPV感染情况及高危型分布的meta分析[D]. 乌鲁木齐: 新疆医科大学, 2015.Xu Y. Meta-analysis of HPV infection and high-risk type distribution in cervical lesions in Xinjiang Province[D]. Wulumuqi: Xinjiang Medical University, 2015. [18] 李翀, 郑旭. 天津地区4232例妇女宫颈HPV感染基因谱分析[J]. 中国妇幼保健, 2015, 30(10): 1571-1573. DOI: 10.7620/zgfybj.j.issn.1001-4411.2015.10.36.Li C, Zheng X. Genomic analysis of cervical HPV infection in 4232 women in Tianjin[J]. Maternal and Child Health Care of China, 2015, 30(10): 1571-1573. DOI: 10.7620/zgfybj.j.issn.1001-4411.2015.10.36. [19] 周小会, 史艳丰, 汪丽杰, 等. 上海地区女性宫颈人乳头状瘤病毒型别分布的Meta分析[J]. 中国妇幼健康研究, 2016, 27(11): 1348-1353. DOI: 10.3969/j.issn.1673-5293.2016.11.018.Zhou XH, Shi YF, Wang LJ, et al. Meta-analysis of cervical human papillomavirus type distribution in Shanghai[J]. Chinese Journal of Woman and Child Health Research, 2016, 27(11): 1348-1353. DOI: 10.3969/j.issn.1673-5293.2016.11.018. [20] 王春霞, 马艳云, 孙涛, 等. 甘肃省妇女子宫颈人乳头瘤病毒感染情况的Meta分析[J]. 中国妇幼保健, 2017, 32(12): 2811-2813. DOI: 10.7620/zgfybj.j.issn.1001-4411.2017.12.103.Wang CX, Ma YY, Sun T, et al. Study on the distribution of human papillomavirus types in cervix among Chinese women: a meta-analysis[J]. Maternal and Child Health Care of China, 2017, 32(12): 2811-2813. DOI: 10.7620/zgfybj.j.issn.1001-4411.2017.12.103. [21] 吕永金, 谢沁玲, 郑宝文, 等. 子宫颈癌筛查大样本数据引发的思考[J]. 中华临床实验室管理电子杂志, 2016, 4(1): 8-12. DOI: 10.3877/cma.j.issn.2095-5820.2016.01.003.Lv YJ, Xie QL, Zheng BW, et al. Insights and thinking from big data of cervical examination and human papillomavirus test[J]. Chin J Clin Lab Mgt(Electronic Edition), 2016, 4(1): 8-12. DOI: 10.3877/cma.j.issn.2095-5820.2016.01.003. [22] 魏丽惠, 赵昀, 沈丹华, 等. 中国子宫颈癌筛查及异常管理相关问题专家共识(一)[J]. 中国妇产科临床杂志, 2017, 18(2): 190-192.Wei LH, Zhao Y, Shen DH, et al. Expert consensus on cervical cancer screening and abnormal management in China (1)[J]. Chin J Clin Obstet Gynecol, 2017, 18(2): 190-192. -





 下载:
下载: