Joint effect of serum C-reactive protein and genetic risk in the pathogenesis of cancer
-
摘要:
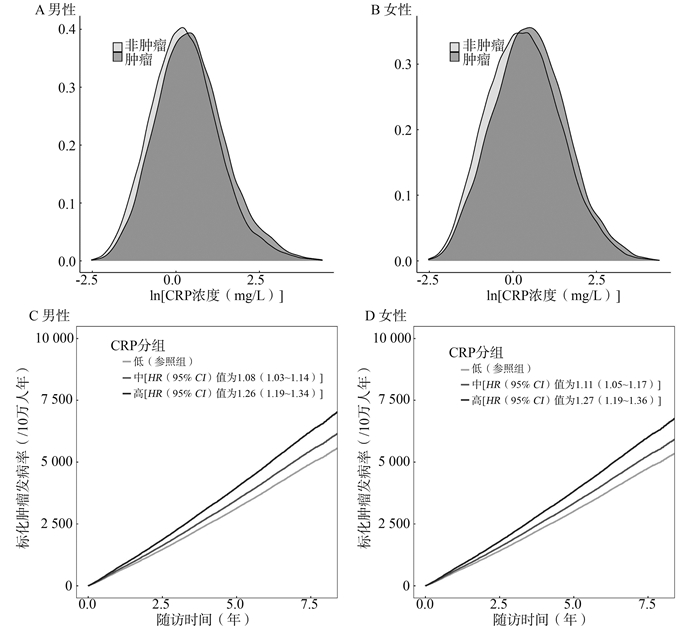
目的 探讨血清C反应蛋白(C-reactive protein, CRP)和遗传风险在恶性肿瘤发病中的联合作用。 方法 基于英国生物样本库(UK Biobank, UKB)以及前期已构建的全恶性肿瘤多基因遗传风险评分(cancer polygenic risk score, CPRS),将研究对象分为高、中、低三个遗传风险组,同时按照血清CRP浓度的自然对数值大小将研究对象分为高、中、低三个水平组。采用Cox比例风险模型,分析不同遗传风险组中,血清CRP水平与恶性肿瘤发病风险的关联。 结果 共纳入420 940位研究对象,包括男性192 942名(45.84%),女性227 998名(54.16%)。血清CRP水平与多种恶性肿瘤的发病风险均存在统计学关联,随着血清CRP水平的升高,男性和女性整体恶性肿瘤的发病风险均增加(男性:HR=1.09, 95% CI: 1.07~1.11; 女性:HR=1.09, 95% CI: 1.07~1.11);在低遗传风险组中,高水平CRP与恶性肿瘤发病风险关联效应更强(男性:HR=1.38;女性:HR=1.46);在高遗传风险组中,高水平CRP与恶性肿瘤发病风险关联效应较弱(男性:HR=1.07;女性:HR=1.17),呈负向交互作用。 结论 高血清CRP水平可增加恶性肿瘤发病风险,其在低遗传风险人群中可能具有更强的效应。 Abstract:Objective To explore the joint effect of serum C-reactive protein (CRP) and genetic risk in the pathogenesis of cancer. Methods Based on UK Biobank data and the cancer polygenic risk score (CPRS) constructed previously, subjects were assigned into low, intermediate, and high genetic risk groups according to CPRS and were assigned into low, intermediate, and high groups based on natural logarithm of CRP. Cox proportional hazard model was used to test the association between serum CRP level and the risk of cancer in different genetic risk groups. Results A total of 420 940 subjects including 192 942 (45.84%) men and 227 998 (54.16%) women were included. The level of serum CRP was statistically associated with the risk of multiple cancers. High level of serum CRP was associated with an increased risk of overall cancer in male and female (male: HR=1.09, 95% CI: 1.07-1.11; female: HR=1.09, 95% CI: 1.07-1.11). The effect size of CRP on cancer risk was stronger in low genetic risk group (male: HR=1.38; female: HR=1.46) compared to that of high genetic risk group (male: HR=1.07; female: HR=1.17). There was a negative interaction between CRP and genetic risk in cancer. Conclusions High level of serum CRP can increase the cancer risk. Serum CRP level may have a stronger effect in low genetic risk population. -
Key words:
- Cancer /
- C-reactive protein /
- Polygenic risk score /
- Interaction
-
表 1 血清CRP水平与恶性肿瘤发病风险的关联(按遗传风险分层)
Table 1. The association between CRP level in serum and the risk of overall cancer (stratified by genetic risk)
性别 低遗传风险 中遗传风险 高遗传风险 低CRP 中CRP 高CRP 低CRP 中CRP 高CRP 低CRP 中CRP 高CRP 男性 病例/人年 286/55 241 1 130/159 995 481/51 188 1 135/162 261 4 313/477 270 1 888/156 914 618/53 614 2 134/155 942 817/52 460 HR(95% CI)值 1.00 1.17(1.02~1.34) 1.38(1.18~1.61) 1.00 1.10(1.03~1.17) 1.33(1.23~1.43) 1.00 1.02(0.93~1.12) 1.07(0.96~1.20) P值 0.020 <0.001 0.006 <0.001 0.680 0.208 女性 病例/人年 287/63 680 1 202/191 477 513/62 787 1 124/194 155 4 265/567 778 1747/187 793 520/63 985 1 874/185 814 736/63 371 HR(95% CI)值 1.00 1.19(1.04~1.36) 1.46(1.24~1.71) 1.00 1.10(1.03~1.18) 1.27(1.17~1.38) 1.00 1.08(0.98~1.20) 1.17(1.03~1.33) P值 0.010 <0.001 0.005 <0.001 0.136 0.015 -
[1] International Association of Cancer Registries. Cancer today[EB/OL]. (2020-09)[2021-08-24]. http://gco.iarc.fr/today/home. [2] Shen J, Hernandez D, McNeill LH, et al. Associations of serum CRP levels with demographics, health behaviors, and risk of can-cer among the Mexican American Mano A Mano Cohort[J]. Cancer Epidemiol, 2019, 60: 1-7. DOI: 10.1016/j.canep.2019.03.001. [3] Eklund CM. Proinflammatory cytokines in CRP baseline regulation[J]. Adv Clin Chem, 2009, 48: 111-136. DOI: 10.1016/s0065-2423(09)48005-3. [4] Van'T KC, Ridker PM, Hjortnaes J, et al. The relation between systemic inflammation and incident cancer in patients with stable cardiovascular disease: a cohort study[J]. Eur Heart J, 2019, 40(48): 3901-3909. DOI: 10.1093/eurheartj/ehz587. [5] Morrison L, Laukkanen JA, Ronkainen K, et al. Inflammatory biomarker score and cancer: a population-based prospective cohort study[J]. BMC Cancer, 2016, 16: 80. DOI: 10.1186/s12885-016-2115-6. [6] Duprez DA, Otvos J, Sanchez OA, et al. Comparison of the predictive value of GlycA and other biomarkers of inflammation for total death, incident cardiovascular events, noncardiovascular and noncancer inflammatory-related events, and total cancer events[J]. Clin Chem, 2016, 62(7): 1020-1031. DOI: 10.1373/clinchem.2016.255828. [7] Buniello A, MacArthur J, Cerezo M, et al. The NHGRI-EBI GWAS catalog of published genome-wide association studies, targeted arrays and summary statistics 2019[J]. Nucleic Acids Res, 2019, 47(D1): D1005-D1012. DOI: 10.1093/nar/gky1120. [8] Zhu M, Wang T, Huang Y, et al. Genetic risk for overall cancer and the benefit of adherence to a healthy lifestyle[J]. Cancer Res, 2021. DOI: 10.1158/0008-5472.CAN-21-0836. [9] Blechter B, Wong J, Agnes HC, et al. Sub-multiplicative interaction between polygenic risk score and household coal use in relation to lung adenocarcinoma among never-smoking women in Asia[J]. Environ Int, 2021, 147: 105975. DOI: 10.1016/j.envint.2020.105975. [10] Huang Y, Zhu M, Ji M, et al. Air pollution, genetic factors and the risk of lung cancer: a prospective study in the UK Biobank[J]. Am J Respir Crit Care Med, 2021. DOI: 10.1164/rccm.202011-4063OC. [11] Jin G, Lv J, Yang M, et al. Genetic risk, incident gastric cancer, and healthy lifestyle: a meta-analysis of genome-wide association studies and prospective cohort study[J]. Lancet Oncol, 2020, 21(10): 1378-1386. DOI: 10.1016/S1470-2045(20)30460-5. [12] Bycroft C, Freeman C, Petkova D, et al. The UK Biobank resource with deep phenotyping and genomic data[J]. Nature, 2018, 562(7726): 203-209. DOI: 10.1038/s41586-018-0579-z. [13] Caul S, Broggio J. Cancer registration statistics, England[EB/OL]. (2019-04-26)[2021-08-24]. https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/datasets/cancerregistrationstatisticscancerregistrationstatisticsengland. [14] Heinzl H, Kaider A. Gaining more flexibility in Cox proportional hazards regression models with cubic spline functions[J]. Comput Methods Programs Biomed, 1997, 54(3): 201-208. DOI: 10.1016/s0169-2607(97)00043-6. [15] Michels N, van Aart C, Morisse J, et al. Chronic inflammation towards cancer incidence: a systematic review and meta-analysis of epidemiological studies[J]. Crit Rev Oncol Hematol, 2021, 157: 103177. DOI: 10.1016/j.critrevonc.2020.103177. [16] Mantovani A, Allavena P, Sica A, et al. Cancer-related inflammation[J]. Nature, 2008, 454(7203): 436-444. DOI: 10.1038/nature07205. [17] Lauby-Secretan B, Scoccianti C, Loomis D, et al. Body fatness and cancer--viewpoint of the IARC Working Group[J]. N Engl J Med, 2016, 375(8): 794-798. DOI: 10.1056/NEJMsr1606602. [18] Jayedi A, Emadi A, Shab-Bidar S. Dietary inflammatory index and site-specific cancer risk: a systematic review and dose-response meta-analysis[J]. Adv Nutr, 2018, 9(4): 388-403. DOI: 10.1093/advances/nmy015. [19] Platz EA, Sutcliffe S, De Marzo AM, et al. Intra-individual variation in serum C-reactive protein over 4 years: an implication for epidemiologic studies[J]. Cancer Causes Control, 2010, 21(6): 847-851. DOI: 10.1007/s10552-010-9511-z. -





 下载:
下载: