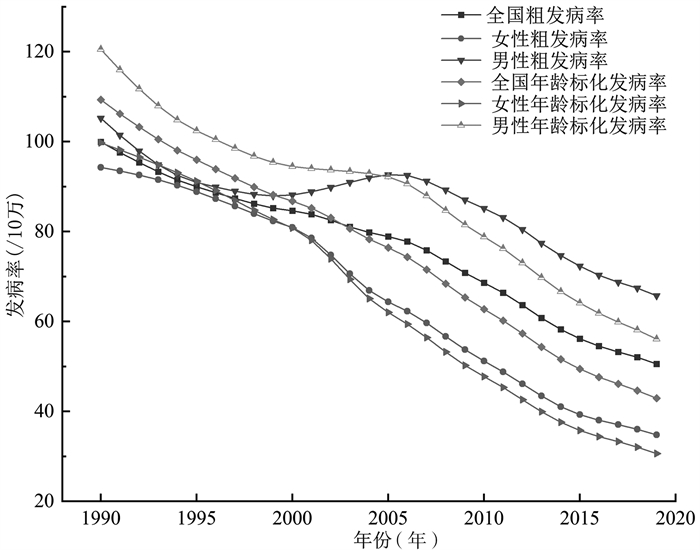
Trend of tuberculosis incidence in China from 1990 to 2019 based on the age-period-cohort model
-
摘要:
目的 分析1990―2019年中国结核病发病趋势并探讨年龄、时期、队列对结核病发病风险的影响。 方法 收集全球健康数据交换数据库中0~ < 95岁中国居民结核病发病数据,采用Joinpoint回归模型分析1990―2019年中国居民结核病发病率的变化趋势,采用年龄-时期-队列模型来分析影响中国结核病发病风险的年龄效应、时期效应和队列效应。 结果 1990―2019年,全国、男性、女性的结核病标化发病率均呈下降趋势,男性、女性年龄标化发病率分别从1990年的120.56/10万和99.75/10万下降至2019年的56.08/10万和30.60/10万,年平均下降速度分别为2.60%和3.98%。年龄-时期-队列模型分析结果显示,1990―2019年中国结核病发病率的年龄效应总体上随年龄的增加而增加,在90~ < 95岁发病风险达到最大,男性和女性的RR值分别为2.50(95% CI:2.33~2.69)和1.93(95% CI:1.76~2.12);时期效应随着时间的推移发病风险逐渐下降,发病风险RR值从1990年的[男性:1.13(95% CI:1.08~1.17);女性:1.58(95% CI:1.51~1.65)]降至2019年的[男性:0.80(95% CI:0.76~0.83);女性:0.61(95% CI:0.57~0.65)];队列效应显示,出生越晚的人发病风险越小。 结论 1990―2019年中国居民结核病发病率呈现下降趋势,结核病发病风险总体上随着年龄的增加而增加,越早出生的人发病风险越高。建议重点对婴幼儿、大学生、男性、老年等群体进行结核病筛查,全国各大高校多开展结核病健康知识讲座,相关政府部门应该利用多种途径给群众宣传结核病健康知识。 -
关键词:
- 结核病 /
- 发病率 /
- 变化趋势 /
- 年龄-时期-队列模型
Abstract:Objective To analyze the trend of tuberculosis incidence in China in 1990-2019 and to explore the impact of age, period and cohort on tuberculosis risk. Methods The global health data exchange database was used to collect tuberculosis incidence data from Chinese residents aged 0- < 95 years old. Joinpoint regression was used to analyze the changing trend of tuberculosis incidence in China from 1990 to 2019. The age-period-cohort model was used to analyze the age effect, period effect and cohort effect on the risk of tuberculosis in China. Results From 1990 to 2019, the standardized incidence of tuberculosis showed a downward trend in the whole population and in the subgroups of males and females. The age-standardized incidence rate decreased from 120.56/100 000 and 99.75/100 000 in 1990 to 56.08/100 000 and 30.60/100 000 in 2019, with an average annual decline rate of 2.60% and 3.98%, respectively. The results of the age-period-cohort model analysis showed that the age effect of tuberculosis incidence in China increased with age from 1990 to 2019, and reached the highest risk at the age of 90- < 95 years old. The RR of males and females were 2.50 (95% CI: 2.33-2.69) and 1.93 (95% CI: 1.76-2.12), respectively. The period effect gradually decreased with the passage of time, and the RR value of incidence risk decreased from [male: 1.13 (95% CI: 1.08-1.17); female: 1.58 (95% CI: 1.51-1.65)] in 1990 to [male: 0.80 (95% CI: 0.76-0.83); female: 0.61 (95% CI: 0.57-0.65)] in 2019. The cohort effect showed that people who were born later have a lower risk of developing the disease. Conclusions The incidence of tuberculosis in China showed a downward trend from 1990 to 2019. On the whole, the risk of tuberculosis increased with the increase in age. The farther away from the contemporary period, the higher the risk of people being born earlier. It is suggested that TB screening should be focused on infants, college students, men, the elderly, and other groups. Colleges and universities across the country should carry out more lectures on TB health knowledge, and relevant government departments should use a variety of ways to publicize TB health knowledge to the public. -
Key words:
- Tuberculosis /
- Incidence /
- Changing trend /
- Age-period-cohort model
-
表 1 1990―2019年中国结核病ASIR的变化趋势
Table 1. Changing trend of ASIR of tuberculosis in China from 1990 to 2019
年份(年) ASIR(/10万) APC(%, 95% CI)值 AAPC(%, 95% CI)值 t值 P值 1990年 2019年 全国 109.31 42.92 -3.16(-3.23~-3.09) -88.032 < 0.001 1990―1994 -2.62(-2.76~-2.47) 1995―1999 -1.92(-2.05~-1.78) 2000―2004 -2.64(-2.82~-2.46) 2005―2009 -4.18(-4.36~-3.99) 2010―2014 -4.84(-5.14~-4.54) 2015―2019 -3.35(-3.54~-3.16) 男性 120.56 56.08 -2.60(-2.64~-2.55) -105.012 < 0.001 1990―1994 -3.50(-3.64~-3.37) 1995―1999 -1.80(-1.93~-1.67) 2000―2004 -0.61(-0.67~-0.54) 2005―2009 -3.58(-3.71~-3.45) 2010―2014 -4.23(-4.44~-4.03) 2015―2019 -3.23(-3.36~-3.09) 女性 99.75 30.60 -3.98(-4.16~-3.80) -42.815 < 0.001 1990―1995 -1.75(-2.04~-1.46) 1995―1999 -2.52(-2.79~-2.24) 2000―2004 -6.01(-7.12~-4.89) 2005―2009 -4.63(-5.78~-3.48) 2010―2014 -5.56(-5.72~-5.41) 2015―2019 -3.70(-4.10~-3.31) -
[1] Buzic I, Giuffra V. The paleopathological evidence on the origins of human tuberculosis: a review[J]. J Prev Med Hyg, 2020, 61(1 Suppl 1): E3-E8. DOI: 10.15167/2421-4248/jpmh2020.61.1s1.1379. [2] Wang LX, Zhang H, Ruan YZ, et al. Tuberculosis prevalence in China, 1990-2010: a longitudinal analysis of national survey data[J]. Lancet, 2014, 383(9934): 2057-2064. DOI: 10.1016/S0140-6736(13)62639-2. [3] Zuo ZB, Wang MC, Cui HZ, et al. Spatiotemporal characteristics and the epidemiology of tuberculosis in China from 2004 to 2017 by the nationwide surveillance system[J]. BMC Public Health, 2020, 20(1): 1284. DOI: 10.1186/s12889-020-09331-y. [4] 任坦坦, 陆普选, 邓国防, 等. 2020 WHO全球结核报告: 全球与中国关键数据分析[J]. 新发传染病电子杂志, 2020, 5(4): 280-284. DOI: 10.19871/j.cnki.xfcrbzz.2020.04.015.Ren TT, Lu PX, Deng GF, et al. 2020 WHO tuberculosis report: key data for China and the whole world[J]. Electronic Journal of Emerging Infectious Diseases, 2020, 5(4): 280-284. DOI: 10.19871/j.cnki.xfcrbzz.2020.04.015. [5] WHO. Global tuberculosis report 2021[EB/OL]. (2021-10-14)[2021-10-31]. https://www.who.int/publications/digital/global-tuberculosis-report-2021. [6] Meira KC, Silva GWDS, dos Santos J, et al. Analysis of the effects of the age-period-birth cohort on cervical cancer mortality in the Brazilian Northeast[J]. PLoS One, 2020, 15(2): e0226258. DOI: 10.1371/journal.pone.0226258. [7] GBD 2019 Diseases and Injuries Collaborators. Global burden of 369 diseases and injuries in 204 Countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019[J]. Lancet, 2020, 396(10258): 1204-1222. DOI: 10.1016/S0140-6736(20)30925-9. [8] Zhou M, Wang H, Zeng X, et al. Mortality, morbidity, and risk factors in China and its provinces, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017[J]. Lancet, 2019, 394(10204): 1145-1158. DOI: 10.1016/S0140-6736(19)30427-1. [9] 屈彦, 王天一, 杨津, 等. GBD数据库的数据提取方法与流程[J]. 中国循证心血管医学杂志, 2019, 11(9): 1043-1046. DOI: 10.3969/j.issn.1674-4055.2019.09.04.Qu Y, Wang TY, Yang J, et al. GBD database application and data extraction methods and processes[J]. Chin J Evid Based Cardiovasc Med, 2019, 11(9):1043-1046. DOI: 10.3969/j.issn.1674-4055.2019.09.04.DOI:10.3969/j.issn.1674-4055.2019.09.04. [10] GBD 2019 Demographics Collaborators. Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 Countries and territories, 1950-2019: a comprehensive demographic analysis for the Global Burden of Disease Study 2019[J]. Lancet, 2020, 396(10258): 1160-1203. DOI: 10.1016/S0140-6736(20)30977-6. [11] 曾四清. Joinpoint回归模型及其在传染病流行趋势分析中的应用[J]. 中国卫生统计, 2019, 36(5): 787-791. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGWT201905044.htmZeng SQ. Joinpoint regression model and its application in epidemic trend analysis of infectious diseases[J]. Chin J Heal Stat, 2019, 36(5): 787-791. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGWT201905044.htm [12] Yang Y, Fu WJ, Land KC. A methodological comparison of age-period-cohort models: the intrinsic estimator and conventional generalized linear models[J]. Sociol Methodol, 2004, 34(1): 75-110. DOI: 10.1111/j.0081-1750.2004.00148.x. [13] Yang Y. Trends in U.S. adult chronic disease mortality, 1960-1999: age, period, and cohort variations[J]. Demography, 2008, 45(2): 387-416. DOI: 10.1353/dem.0.0000. [14] Donald PR, Marais BJ, Barry CE 3rd. Age and the epidemiology and pathogenesis of tuberculosis[J]. Lancet, 2010, 375(9729): 1852-1854. DOI: 10.1016/S0140-6736(10)60580-6. [15] Fernandes P, Ma Y, Gaeddert M, et al. Sex and age differences in Mycobacterium tuberculosis infection in Brazil[J]. Epidemiol Infect, 2018, 146(12): 1503-1510. DOI: 10.1017/S0950268818001450. [16] 姚晶, 顾凯侃, 李智红, 等. 2014-2019年上海市静安区老年与非老年肺结核流行特征对比分析[J]. 中国防痨杂志, 2020, 42(12): 1323-1328. DOI: 10.3969/j.issn.1000-6621.2020.12.014.Yao J, Gu KK, Li ZH, et al. A comparative analysis of the epidemic characteristics of tuberculosis in elderly and non-elderly in Jing'an District, Shanghai from 2014 to 2019[J]. Chin J Antituberc, 2020, 42(12): 1323-1328. DOI: 10.3969/j.issn.1000-6621.2020.12.014. [17] Gavazzi G, Krause KH. Ageing and infection[J]. Lancet Infect Dis, 2002, 2(11): 659-666. DOI: 10.1016/s1473-3099(02)00437-1. [18] Fischer J, Jung N, Robinson N, et al. Sex differences in immune responses to infectious diseases[J]. Infection, 2015, 43(4): 399-403. DOI: 10.1007/s15010-015-0791-9. [19] 何志青, 胡贵方, 资青兰, 等. 影响男性肺结核发病的相关因素探讨[J]. 实用医学杂志, 2012, 28(23): 3905-3907. DOI: 10.3969/j.issn.1006-5725.2012.23.019.He ZQ, Hu GF, Zi QL, et al. Study on the related factors affecting the incidence of male pulmonary tuberculosis[J]. The J Pract Med, 2012, 28(23): 3905-3907. DOI: 10.3969/j.issn.1006-5725.2012.23.019. [20] Carvalho ACC, Cardoso CAA, Martire TM, et al. Epidemiological aspects, clinical manifestations, and prevention of pediatric tuberculosis from the perspective of the End TB Strategy[J]. J Bras Pneumol, 2018, 44(2): 134-144. DOI: 10.1590/s1806-37562017000000461. [21] 王文琴, 梁日成, 余小华, 等. 大学生群体肺结核患病的流行病学研究, 以广西大学大学生为研究案例[J]. 基因组学与应用生物学, 2017, 36(6): 2248-2254. DOI: 10.13417/j.gab.036.002248.Wang WQ, Liang RC, Yu XH, et al. Epidemiological study of pulmonary tuberculosis among college students, case study of students in Guangxi University[J]. Genom Appl Biol, 2017, 36(6): 2248-2254. DOI: 10.13417/j.gab.036.002248. [22] 陆伟, 周扬, 刘剑君. 新中国成立70年来我国结核病防治工作的进展与成就[J]. 中华疾病控制杂志, 2019, 23(7): 754-757, 762. DOI: 10.16462/j.cnki.zhjbkz.2019.07.003.Lu W, Zhou Y, Liu JJ. The progress and achievements of tuberculosis control in China since 1949[J]. Chin J Dis Control Prev, 2019, 23(7): 754-757, 762. DOI: 10.16462/j.cnki.zhjbkz.2019.07.003. [23] Davenport RJ. Year of birth effects in the historical decline of tuberculosis mortality: a reconsideration[J]. PLoS One, 2013, 8(12): e81797. DOI: 10.1371/journal.pone.0081797. [24] 吴影桃, 柳莉, 严翠婷, 等. 基于微信平台健康教育对社区非肺结核人群普及预防肺结核知识的效果研究[J]. 中国医药指南, 2020, 18(13): 294-295. DOI: 10.15912/j.cnki.gocm.2020.13.140.Wu YT, Liu L, Yan CT, et al. Study on the effect of health education based on wechat platform on the popularization of tuberculosis prevention knowledge among non tuberculosis population in community[J]. Guide of China Medicine, 2020, 18(13): 294-295. DOI: 10.15912/j.cnki.gocm.2020.13.140. [25] 余巧林, 雷丽梅, 万彬, 等. 结核病患者健康素养与结核病防治核心知识和社会支持的相关性[J]. 中国防痨杂志, 2020, 42(11): 1227-1231. DOI: 10.3969/j.issn.1000-6621.2020.11.015.Yu QL, Lei LM, Wan B, et al. Correlation between health literacy of tuberculosis patients and core knowledge and social support of tuberculosis control[J]. Chin J Antitubercul, 2020, 42(11): 1227-1231. DOI: 10.3969/j.issn.1000-6621.2020.11.015. [26] Wang LQ, Wang WB. Temporal trends in notification and mortality of tuberculosis in China, 2004-2019: a joinpoint and age-period-cohort analysis[J]. Int J Environ Res Public Health, 2021, 18(11): 5607. DOI: 10.3390/ijerph18115607. -





 下载:
下载: